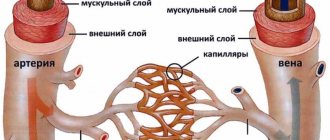
Cortical atrophy of the brain is a devastating, irreversible change that most often affects people between 50 and 55 years of age, although there are cases of cortical atrophy in newborn infants. Pathological disorders, as a rule, manifest themselves in the frontal lobes of the brain, which are responsible for the thinking process, human behavior, and control. The disease progresses slowly with a gradual increase in the main symptoms, which ultimately leads to the emergence and development of senile dementia.
What it is?
The main organ of humans is the brain, which includes many nerve cells. Atrophic changes in its cortex lead to the gradual death of nerve cells, and mental abilities fade over time. The lifespan of a person depends on the age at which this pathology began to develop.
You will be interested in: “Grandaxin”: analogues and substitutes, instructions for use, reviews
Changes in behavior are noticeable in almost all older people, but due to their slow development, these signs of decline are not considered pathological. Many older people are unable to respond to environmental changes in the same way as they did at a young age. In the elderly, intelligence decreases, but these changes do not cause neurology, psychopathy and dementia.
With cerebral atrophy of the brain, brain cells gradually die and nerve endings die. This condition is considered a pathology in which changes occur in the structure of the hemispheres. There is also a smoothing of the convolutions, a decrease in the volume and weight of this organ. The frontal lobes are more often destroyed, which causes a decrease in intelligence and behavioral deviations.
Clinical symptoms of brain atrophy
The manifestations of pathology are largely determined by the causes and provoking factors. Most older people have dementia, frontal lobe syndrome, and internal multiple organ pathology.
How does frontal lobe syndrome manifest?
- Lack of appetite;
- Loss of memory, intellectual activity;
- Frequent emotional breakdowns;
- Lack of communication with surrounding people;
- Irritability;
- Lack of self-criticism.
Psychoorganic syndrome is accompanied by cerebroasthenic disorders, affective disorders, and amnesia.
The patient lacks an adequate assessment of surrounding events and self-criticism. Primitive thinking appears, a one-sided representation of the essence of the detail. Speech reserve decreases, paramnesia appears.
Concomitant affective disorders lead to depressive syndrome and inadequate mental state. Tearfulness, touchiness, irritability, unreasonable aggression are typical manifestations of pathology.
Congenital
These include:
- genetic factor;
- intrauterine infectious diseases;
- genetic mutations.
One of the genetic diseases that affects the cerebral cortex is Pick's disease. It is usually observed in middle-aged people, which manifests itself in the gradual damage of frontal and temporal neurons. The disease can develop rapidly and after 5-6 years leads to death.
Infection of a child during pregnancy also leads to the destruction of various organs, including the brain. For example, infection with toxoplasmosis in the early stages of gestation leads to damage to the nervous system of the fetus. After this, babies usually do not survive or are born with congenital abnormalities and mental retardation.
Causes
The following reasons can provoke the death of the cerebral cortex:
These are immediate causes that can disrupt the nutrition of nerve cells in the brain. There are also indirect factors that, although they do not cause atrophy, provoke the development of the main causes:
- smoking;
- high blood pressure;
- lack of intellectual load on the cognitive abilities of the brain.
Atrophic changes in the cerebellum
The area of cell destruction is located in the cerebellum, the coordination center. The disease is accompanied by changes in muscle tone, the inability to hold the head straight and impaired coordination of body position.
People with cerebellar atrophy lose the ability to care for themselves: movements are often uncontrollable, and limbs tremble when performing actions.
Speech is disrupted: it slows down and becomes chanted. In addition to specific symptoms, destruction of the cortex causes headaches, dizziness, drowsiness and apathy.
As atrophy occurs, pressure inside the skull rises. Often the cranial nerves are paralyzed, which can immobilize the eye muscles. Basal reflexes also disappear.
Cortical atrophy
Pathology is manifested by personality degradation. A sick person loses the ability to control his behavior, criticism of his condition decreases
Cognitive abilities decrease: thinking, memory, attention - the quantitative properties of these mental processes (speed, pace, concentration, volume) are disrupted. Memory regresses according to Ribot's law: first, recent events are forgotten, then events of several years ago, after which memories of ten years ago and early youth are forgotten
Atrophy of the cortex entails the development of infantilism. The patient’s psyche degenerates to the previous stage of development: “adulthood” disappears, decisions are made with difficulty, childish qualities appear in the personality pattern. Interest in social issues is lost, and hobbies include entertainment. Emotions also degrade: egocentrism, capriciousness, restlessness develop
People with an atrophied cortex do not want to take into account the interests and opinions of family, team or friends
Intellectual deficiency is increasing. With the dynamics of atrophy, the ability for abstract logical thinking decreases. Difficulties in understanding professional terminology, hampering the ability to solve standard and everyday problems.
Violation of trophism affects the sphere of higher skills. Patients forget how to tie shoelaces and cook food. Musicians forget chords, artists forget how to use a brush correctly, writers forget what order the words in a sentence should be in.
As the pathology deepens, patients lose the ability to perform basic actions: brushing their teeth, holding a spoon, looking both ways when crossing the road.
The outcome of the disease is social degradation, deep infantilism and dementia. Such people are hospitalized in a psychiatric hospital and then sent to boarding schools.
Generalized cerebral atrophy
This is a systemic progressive atrophy of all parts of the human telencephalon. This form of pathology includes atrophy of the cortex and cerebellum. The brain decreases in size over time. As it progresses, most intellectual abilities are lost.
The severity of atrophy is determined by its degree:
Brain nutrition disorder 1st degree.
Characterized by minimal manifestations of the disease
People become forgetful, think more slowly, their attention is distracted, and their vocabulary decreases. Proposals are hard to write
Difficulties arise in choosing words.
The first degree is most often asymptomatic. The first signs are regarded as fatigue, lack of sleep, stress. Hypochondriacal patients begin to look for illnesses within themselves that could provoke something wrong.
By consulting a doctor, you can slow down the dynamics of the disease, prevent the progression of the clinical picture and partially restore impaired functions.
The clinical picture is characterized by an increase in intellectual defects. The ability to memorize new information deteriorates, it is more difficult to master new skills
Signs of degree 2: decreased attention, deterioration of short-term memory, inability to make decisions independently
Purchased
You will be interested in: The drug "Novopassit": analogues, indications, instructions for use, reviews, contraindications and side effects
There are also acquired reasons. Brain atrophy can occur from:
- Drinking alcohol and smoking. This causes cerebral vascular spasm, resulting in oxygen starvation. Because of this, white matter cells cannot receive enough nutrients, causing them to die.
- Infectious diseases that affect nerve cells - meningitis, rabies, polio.
- Injuries, concussions and mechanical damage.
- Severe form of renal failure. This causes general intoxication of the body, which causes metabolic disorders.
- Hydrocephalus disorders. This phenomenon manifests itself in an increase in the subarachnoid space and ventricles.
- Chronic ischemia, which leads to vascular damage and low supply of nutrients to neural connections.
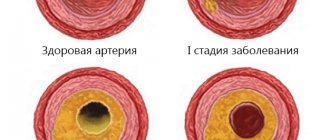
- Atherosclerosis, which manifests itself in a narrowing of the lumen of veins and arteries, which increases intracranial pressure and creates a risk of stroke.
Atrophy of the cerebral cortex can occur due to insufficient intellectual and physical activity, lack of a balanced diet and poor lifestyle.
Classification
The division of the pathological process is carried out according to several criteria. The main and most common is the type of disorder.
Primary form
Develops against the background of genetic abnormalities and defects. It is relatively rare, but presents enormous difficulties from a therapeutic point of view.
Recovery is impossible in principle; all that remains is to reduce the intensity of the symptoms. In this case, the prognosis is always unfavorable; the patient plunges into a state of deep disability in a matter of years, then dies.
The trigger mechanism for the onset of cerebral atrophy is injury, past infections, and other negative factors.
Secondary form
Seen much more often. The intensity of symptoms, the path and nature of the course, and other points depend on the specific cause.
In some cases, it is possible to quite successfully stabilize the development of the pathological process, maintaining the patient in a normal state for many years.
Degrees of impairment
The second method of classification is fractional, based on the degree of involvement of brain structures in the disorder.
- Cortical atrophy. Characterized by local changes in nerve tissue. As a rule, atrophy of the cerebral cortex occurs, and most often at the level of the frontal lobes. A person quickly falls into inadequacy, loses the ability for emotional and mental self-regulation and becomes a burden for relatives.
- Multisystem form. It's diffuse. Slightly less common. A characteristic feature is the development of a group of foci of atrophy. The process occurs due to genetic abnormalities, congenital factors, injuries, infections. Possible development after a stroke. The treatment does not have much effect.
- Generalized atrophy. An even more pronounced form of the “drying out” process. The entire brain is affected. Mostly begins against the background of current dementia. Senile and other types, including Alzheimer's disease.
Stages of development
Subdivision is also possible according to the stages of development of the disorder. Then they talk about staging the disorder. There are three phases in the development of the problem:
- First. Accompanied by minimal atrophic changes. The patient does not suspect anything yet. However, neurological disorders are already present. The first signs include: decreased quality and productivity of thinking, impaired memory, and behavior. The patient is still able to be aware of himself and control his own behavior.
- Second stage. Accompanied by much more pronounced deviations. They become noticeable at first glance. Problems with thinking and speech are typical. Forgetfulness develops. The fact that the emotional component is preserved is paradoxical. If a person is upset about something, he will quickly forget about it, but the negative affect will remain. Behavior gradually deteriorates. The patient becomes not quite adequate, and eccentric antics are characteristic.
- The third stage is determined by the total degradation of personality. The functions of higher nervous activity are lost. The patient is no longer able to think or act. We depend on the people who look after him.
- Does not speak, reacts poorly to all external stimuli. Doesn't show emotion. There can no longer be a way out of this state. For several years the person continues to function this way. But most often they die faster, from stagnation in the body and complications.
Classifications are used by specialists in different variations. The main task is to most accurately describe the pathological process. Therapy, its quality and the likelihood of effective help depend on understanding the essence of the phenomenon.
Why does the disease develop?
Brain atrophy in adults and children usually develops due to a genetic predisposition to the disease, but acceleration and provocation of neuronal death can occur from various injuries and other factors. Atrophic changes appear in different parts of the cortex and subcortical substance, but with different manifestations of the disease, one clinical picture is observed. Small changes can be stopped and a person’s condition can be improved through medical means and lifestyle changes, but the disease cannot be completely eliminated.
Atrophy of the frontal lobes also develops during intrauterine maturation or prolonged labor due to prolonged oxygen starvation, causing necrotic processes in the cerebral cortex. These children usually die in the womb or are born with noticeable abnormalities. Brain cells are capable of dying due to mutations at the gene level due to the impact of harmful components on the health of a pregnant woman and prolonged intoxication of the fetus. But it could also be a chromosomal malfunction.
Video
The brain regulates the functioning of all organ systems, so any damage to it threatens the normal functioning of the entire body, primarily processes such as thinking, speech and memory. Brain atrophy in young people and adults is a pathological condition in which the death of neurons and loss of connections between them progresses.
The result is a reduction in the brain, a smoothing of the relief of the cerebral cortex and a decrease in function, which is of important clinical significance.
Atrophy of the cerebral cortex most often affects older people, especially women, but it also occurs in newborns. In rare cases, the cause is congenital malformations or birth injuries, then the disease begins to manifest itself in early childhood and leads to death.
Symptoms
Regardless of the causes of the disease, general symptoms of brain atrophy can be identified.
Healthy brain tissue and atrophy
The main symptoms of brain atrophy include:
- Mental disorders.
- Behavioral disorders.
- Decreased cognitive function.
- Memory impairment.
- Changes in motor activity.
Stages of the disease:
The patient leads a normal lifestyle and carries out his previous work without difficulty, if it does not require high levels of intelligence. Mostly nonspecific symptoms are observed: dizziness, headache, forgetfulness, depression and lability of the nervous system. Diagnosis at this stage will help slow down the progression of the disease.
Cognitive function continues to decline, self-control is weakened, and inexplicable and thoughtless actions appear in the patient’s behavior. Possible disturbances in coordination of movements and fine motor skills, spatial disorientation. The ability to work and adaptation to the social environment decline.
As the disease develops, the symptoms of brain atrophy progress: the comprehension of speech decreases, the patient needs the help and care of an outsider. By changing the perception and assessment of events, there are fewer complaints.
At the last stage, the most serious changes in the brain occur: atrophy leads to dementia or dementia. The patient is no longer able to perform simple tasks, form speech, read and write, or use household items. Signs of a mental disorder, changes in gait and impaired reflexes are noticeable to others. The patient completely loses contact with the world and the ability to self-care.
Involvement of the cerebellum in the pathological process leads to significant impairment of speech, coordination of movements and gait, and sometimes hearing and vision. Changes in character and sharp deviations in the psyche indicate a pathological process in the area of the frontal lobes.
Signs of predominant damage to one hemisphere of the cerebral cortex indicate a diffuse nature of atrophy.
Memory impairment is one of the symptoms of brain atrophyCauses
The prerequisites for the development of the disease may be different, but most often the following causes of brain atrophy are identified:
- Hereditary mutations and spontaneous mutagenesis.
- Radiobiological effects.
- Infectious diseases of the central nervous system.
- Dropsy of the brain.
- Pathological changes in cerebral vessels.
- Traumatic brain injuries.
Genetic abnormalities that can cause the disease include Pick's disease, which occurs in old age. The disease progresses over 5-6 years and ends in death.
Radiobiological effects can be caused by exposure to ionizing radiation, although the extent of its negative impact is difficult to assess.
Neuroinfections lead to acute inflammation, after which hydrocephalus develops. The fluid that accumulates in this case has a compressive effect on the cerebral cortex, which is the mechanism of damage. Hydrocele can also be an independent congenital disease.
Cerebrovascular pathologies most often arise as a result of atherosclerosis and arterial hypertension and result in cerebral ischemia. Poor circulation becomes the cause of dystrophic and then atrophic changes.
Signs
What are the signs of brain atrophy? At the initial stage of the disease, the symptoms are hardly noticeable and can only be detected by close people. The patient develops apathy, lack of desires, aspirations, lethargy and indifference. A lack of moral principles and increased sexual activity are often observed.
You may be interested in: Beta-alanine: effects, benefits and harms, features of use
As brain cell death progresses, the following signs are observed:
Then, with atrophy, a deterioration in well-being appears and thought processes decrease. A person does not recognize familiar things and forgets about the rules for their use. Elimination of one's behavioral characteristics causes the appearance of the “mirror” syndrome, in which a person begins to copy other people. Then senile insanity and absolute degradation of personality are observed.
The changes in behavior that have arisen do not allow an accurate diagnosis to be made, so to establish the causes of the changes, a list of studies must be carried out. But thanks to the doctor, it will be possible to determine which part of the brain has undergone destructuring. In case of destruction in the cerebral cortex:
Symptoms of changes in the subcortical substance are determined by the functions that the affected section performs, so limited atrophy has its own characteristics. With necrosis of the tissues of the medulla oblongata, respiratory failure, digestive failure are observed, and the cardiovascular and immune systems suffer.
If damage to the cerebellum is observed, muscle tone is disrupted and coordination of movements is impaired. With the destruction of the midbrain, there is no reaction to external stimuli. When the cells of the intermediate section die, a violation of the body's thermoregulation and a metabolic failure appear.
With damage to the anterior section, all reflexes are lost. When neurons die, the function of independent maintenance of life is lost, which usually leads to death. Often, necrotic changes appear from injury or long-term poisoning by toxins.
Main manifestations
Brain atrophy manifests itself depending on which part of the brain the pathological changes begin in. Gradually, the pathological process ends in dementia.
At the beginning of development, atrophy affects the cerebral cortex. This leads to deviations in behavior, inappropriate and unmotivated actions, and decreased self-criticism. The patient becomes sloppy, emotionally unstable, and depression may develop. The ability to remember and intelligence are impaired, which manifests itself in the early stages.
Gradually the symptoms increase. The patient not only cannot work, but also cannot care for himself. There are significant difficulties with eating and going to the toilet. A person cannot complete these tasks without the help of other people.
The patient stops complaining that his intelligence has deteriorated, since he is unable to evaluate it. If there are no complaints about this problem at all, it means that brain damage has reached the last stage. Loss of orientation in space occurs, amnesia appears, the person cannot say his name or where he lives.
If the disease is hereditary, then brain function deteriorates quite quickly. This takes several years. Damage due to vascular disorders can progress over several decades.
The pathological process develops as follows:
- At the initial stage, changes in the brain are small, so the patient leads a normal lifestyle. In this case, the intellect is slightly impaired, and the person cannot solve complex problems. Your gait may change slightly, and you may experience headaches and dizziness. The patient suffers from a tendency to depression, emotional instability, tearfulness, and irritability. These manifestations are usually attributed to age, fatigue, and stress. If you start treatment at this stage, you can slow down the development of pathology.
- The second stage is accompanied by worsening symptoms. Changes in the psyche and behavior are observed, coordination of movements is impaired. The patient cannot control his actions; his actions lack motive and logic. Moderate development of atrophy reduces working capacity and disrupts social adaptation.
- A severe degree of the disease leads to damage to the entire nervous system, which is manifested by impaired motor skills and gait, loss of the ability to write and read, and perform simple actions. The deterioration of the mental state is accompanied by increased excitability or a complete absence of any desires. The swallowing reflex is impaired, and urinary incontinence is common.
At the last stage, the ability to work and communication with the outside world are completely lost. The person develops permanent dementia and is unable to perform basic activities. Therefore, his loved ones must constantly monitor him.
Severity
According to the international classification, there are different degrees of brain atrophy and locations of pathology. Each stage of treatment for the disease has its own symptoms:
With further development, complete destruction occurs and vital systems fail. At this stage, it is better to hospitalize the patient in a psychiatric clinic, since he is difficult to control.
Depending on the location of the affected cells, there are the following types of ailments:
With moderate brain atrophy, changes in personality will be barely noticeable.
Examples of pathology
The most famous examples of a disease such as bihemispheric cortical atrophy (affecting both hemispheres) are senile dementia and Alzheimer's disease. Only severe types of atrophy lead to complete dementia. Small destructive lesions in the vast majority of cases do not affect mental abilities.
It is important to note that grade 1 cortical atrophy refers exclusively to the destruction of nervous brain tissue after its normal formation. With an initially underdeveloped central nervous system, we cannot talk about cortical atrophy.
In children
Brain atrophy may occur in the child. It can be either congenital or acquired, it all depends on the age at which the disease began to develop. The acquired form appears after 1 year of life. The death of nerve cells in children begins for various reasons, for example, due to a genetic factor, different Rh factors in the mother and baby, infection with neuroinfections in the womb, prolonged fetal hypoxia.
Due to the death of neurons, cystic tumors and atrophic hydrocephalus occur. Based on where the cerebrospinal fluid accumulates, cerebral hydrocele can be internal, external, or mixed. A rapidly developing disease is usually observed in newborns, and this is associated with serious disorders in the brain tissue due to prolonged hypoxia, since the child’s body at this stage needs intensive blood supply, and a lack of nutritional components causes serious consequences.
What should the patient's family do?
The disease progresses and the patient requires care.
The first to appear are problems with swallowing liquid or solid food, independent movement and control of urination and defecation are impaired. Relatives of the patient may encounter the following problems:
- Registration of a disability group;
- Receiving social assistance;
- Finding patient care information.
You can assign the patient to a nursing home, where qualified staff will care for the patient. Boarding houses for people with this disease operate on a paid basis; a day’s stay costs from 1,500 rubles.
Link to a European support group for patients with MSA, as well as stories from the lives of patients in Russian and other languages.
What disorders affect the brain?
Subatrophic changes are precursors to global neuronal death. At this stage, it is necessary to promptly identify brain disease and prevent the rapid development of atrophic processes.
For example, with hydrocephalus of the brain in adults, the voids free from destruction are filled with the resulting cerebrospinal fluid. This type of disease is difficult to diagnose, but with proper therapy it will be possible to delay the development of the disease.
You may be interested in: Upper eyelid blepharoplasty: description of the procedure, pros and cons
Changes in the cortex and subcortex are caused by thromophilia and atherosclerosis, which without treatment lead to hypoxia and insufficient blood supply. As a result, neurons die in the back of the head and parietal part, so treatment is necessary to improve blood circulation.
Treatment with folk remedies
Through herbal remedies, the intensity of the negative manifestations of grade 1 cortical medullary atrophy can be reduced.
Good results will be obtained thanks to the following recipes:
- herbal tea - take motherwort, oregano, horsetail and nettle in equal proportions and brew with boiling water in a thermos; the decoction should be infused at night and drunk three times a day;
- chickweed and rye are brewed in a thermos; it is drunk in unlimited quantities after meals; This tea is especially good for treating post-traumatic areas;
- rosehip, viburnum and barberry - the berries of these plants should be poured with boiling water and left for eight hours; You can drink it like tea in any quantity; If necessary, you can add honey.
Alcoholic atrophy
Brain neurons are very sensitive to the effects of alcohol. The decay products poison the neurons, the destruction of neural connections occurs, and then gradual cell death is observed. This leads to brain atrophy.
As a result, both cortical-subcortical cells and brain stem fibers suffer. Damage to blood vessels occurs, shrinkage of neurons and displacement of their nuclei. In patients with alcoholism, self-esteem disappears and memory deteriorates. If he continues to drink alcohol, this will lead to severe intoxication of the body. And even if a person comes to his senses, Alzheimer’s disease and dementia will still develop in the future.
Causes and signs of brain atrophy
Often, the primary manifestations of a cerebral atrophic disorder are expressed in almost imperceptible deviations in a person’s personal state. However, there are factors that help accelerate the disease process, and they should be eliminated as much as possible to prolong normal physiological well-being.
Signs of atrophy:
- Swallowing reflex and breathing disorders, sleep disturbance;
- Decreased brain activity;
- Vocabulary is significantly depleted. It becomes difficult for the patient and it takes more time to find the necessary words when describing basic desires and things;
- The motor functions and motility of the patient’s entire body deteriorate;
- Self-criticism is completely absent. This is often accompanied by deviation from moral principles.
A person suffering from such a complex disorder needs timely treatment, care and control in order to avoid emergency situations in which he is capable of getting into. A patient with cognitive impairment ceases to recognize familiar objects and cannot remember how to use them. There is also a disturbance in orientation in familiar space associated with changes in memory. Further progression of the pathology can lead to degradation and the onset of complete insanity.
When the first signs of atrophy appear, it is necessary to begin treatment of the patient to maintain the normal functionality of his body and brain activity. If prescribed treatment is refused, pathology and atrophic abnormalities of the brain ultimately lead to death.
Causes of atrophy
The causes of brain atrophy are not fully understood. There are suggestions that the syndrome is genetically determined. Primary reflexes suffer from degeneration and death of central neurons in the brain and spinal cord. With a sharp decrease in blood pressure during the adoption of a vertical position, a weakening of secondary reflexes is observed. The development of abnormalities depends on a number of disorders occurring in the brain. Some serious diseases contribute to the formation and development of atrophy: Parkinson's, Behcet's, Whipple's, Cushing's, Alzheimer's, Gellervorden-Spatz's. Other factors also influence:
- Hydrocephalic disorders;
- Brain injuries;
- Drugs, alcohol abuse and smoking;
- Vascular system disorders;
- Impaired metabolism;
- Infectious lesions;
- Amyotrophic sclerosis.
Multiple system atrophy
This disease is considered progressive. The occurrence of the disease includes 3 different disorders, combined with each other in different ways. But usually such atrophy manifests itself in the form of:
- parsionism;
- destruction of the cerebellum;
- vegetative disorders.
To date, the causes of this disease have not been identified. Diagnosis is made using MRI and clinical examination. Treatment includes supportive care and reduction of symptoms of the disease.
Development mechanisms
The formation of the process is quite complex. There are several points. Generally speaking, it is worth mentioning the following ways:
Congenital genetic abnormalities
They are relatively rare, but among all other causes they carry the greatest danger. It is based on a mutation transmitted with “defective” biological material.
The path of inheritance is not exactly known. However, such violations occur most severely and are difficult to slow down. The progression is extremely rapid/An example is Pick's syndrome.
Attention:
Primary forms of brain atrophy cannot be effectively corrected. All that remains is to fight the symptoms.
Acquired pathological processes
Organic changes. A wider range of possible problems. These include disorders of the cardiovascular system, an increase in intracranial pressure against the background of impaired outflow of cerebrospinal fluid.
This also includes disorders of the brain after trauma. The influence of diseases on the likelihood of developing atrophy is enormous. But no doctor can say exactly what the risks are.
Influence of negative factors from outside
Be it ionizing radiation, exposure to toxic, poisonous components on the body, consumption of large amounts of heavy metal salts. People may encounter similar problems when working in hazardous chemical industries, textile factories, etc.
Such forms of the pathological process are difficult to treat, since the provoking factor rapidly destroys neurons. They cannot be restored. Doctors can only slow down the disorder and rehabilitate the patient.
Regardless of the specific pathogenetic moment, the disease develops according to the same pattern: necrosis (death) of nerve fibers forms in entire clusters - these are atrophic changes in the brain.
How fast depends on the specific clinical case. Neurological deficit begins, brain volume decreases. Ultimately, if nothing is done, the patient falls into a vegetative state and dies.
In all situations, capacity gradually fades away, the personality degrades, which becomes a factor of helplessness and disability. Such a person needs constant care.
Cortical atrophy
Usually this type of disease is observed in older people and appears due to senile changes. It affects the frontal lobes, but the disease can spread to other parts. Signs of the disease do not appear immediately, but the result is a decrease in intelligence and memory, and dementia. An example of the impact of such a disease is Alzheimer's disease. Usually diagnosed using MRI.
With the diffuse spread of the disease, blood flow is disrupted, tissue restoration is suffocated and mental performance is reduced. A disorder of fine motor skills of the hands and coordination of movements also appears; the development of the disease changes the lifestyle and leads to absolute incapacity.
Subatrophy of the brain - the first stage of senile dementia
Before clinical symptoms appear, subatrophic changes develop. There are no external symptoms. The condition is accompanied by a partial decrease in the function of a segment of the hemispheres.
Morphological types of subatrophy:
- Frontal;
- Frontotemporal;
- Parieto-occipital.
The first type is characterized by a decrease in mental activity, loss of speech and motor functions.
Damage to the frontotemporal areas leads to a decrease in a person’s hearing ability, communication functions are lost (difficulty communicating with other people), and the functioning of the cardiovascular system is disrupted.
Subatrophy reduces the volume of gray and white matter. Disturbances in conduction and motor function and fine motor activity occur.
Cerebellar atrophy
With this disease, Fr. is also affected. The first symptoms of the disease appear in the form of incoordination of movements, paralysis and speech impairment. With changes in the cerebellar cortex, vascular atherosclerosis and brain stem tumors, infectious diseases, vitamin deficiency and metabolic disorders usually develop.
Cerebellar atrophy manifests itself as:
- speech and fine motor impairments;
- headache;
- nausea, vomiting;
- decreased hearing acuity;
- visual disorders;
- reduction in the mass and volume of the cerebellum.
Treatment involves blocking the signs of the disease with antipsychotics, restoring metabolism, and using cytostatics for tumors. It is possible to eliminate the formations using a surgical method.
Therapy of atrophic pathology of the brain and prognosis of the disease
Drug treatment of atrophic brain pathology involves the use of the following groups of drugs:
- Drugs that improve brain metabolism and blood circulation in it (nootropic drugs). The most prominent representatives of this pharmacological group are: piracetam, Cerepro, Ceraxon, Cerebrolysin. Their administration leads to a significant improvement in the patient’s thinking abilities.
- Antioxidants (mexidol). They have a stimulating effect on regeneration processes, slow down atrophy, help increase metabolic rate, and counteract oxygen free radicals.
- Drugs that improve blood microcirculation. The most commonly prescribed drug is trental (pentoxifylline). The drug has a vasodilating effect, increases the lumen of capillaries, improves blood microcirculation and gas exchange through the vascular wall.
Some signs of cortical atrophy require symptomatic therapy. For headaches, patients are recommended to take non-steroidal anti-inflammatory drugs.
In addition to the use of medication, it is necessary to monitor the patient’s neuropsychic state. Moderate physical activity, daily walks in the fresh air, and self-care procedures are recommended. If the patient is in a neurasthenic state, the use of mild sedatives is indicated.
Diagnostics
The disease is diagnosed by instrumental analysis methods. Using magnetic resonance imaging (MRI), it will be possible to examine in detail changes in the cortical and subcortical substance. Based on the completed images, an accurate diagnosis is made in the early stages of the disease.
Thanks to computed tomography, it is possible to examine vascular lesions after a stroke and establish the causes of hemorrhage, determine the area of cystic formations, which disrupts the normal blood supply to tissues. Multislice tomography is considered a new method of research, with the help of which it will be possible to detect the disease at the initial stage.
Focal cortical atrophies (FCAs) are rare degenerative diseases of the nervous system associated with selective atrophy of individual lobes of the cerebral cortex [1, 2, 4]. Due to the lack of epidemiological studies, their true frequency is unknown. PKA belongs to the class of tauopathies, as they develop due to the pathological accumulation of fragments of phosphorylated t-protein in neurons of the parieto-occipital and temporal lobes. As a result, damage to cell membranes, an increase in the content of intracellular calcium, disturbances in the functioning of mitochondria of the respiratory chain and, as a consequence, apoptosis of neurons are observed [7]. The formation of various FKA phenotypes is associated with a certain anatomical dysfunction of t-immunoreactive structures, the ultrastructure of t-filaments and various haplotypes of the t-protein gene [8]. The causes of selective atrophy of individual areas of the cerebral cortex are unclear. The clinical spectrum of FKA includes posterior cortical atrophy and primary progressive isolated aphasia (ICD-10 G31.0) [1]. The nosological status of FKA has not been definitively determined. Thus, a number of researchers [3, 5, 10] classify them as atypical forms of Alzheimer’s disease or corticobasal degeneration. The extreme rarity of FCA explains significant difficulties in diagnosing this pathology in the daily practice of neurologists. Often, patients with FCA come to the attention of doctors of other specialties (ophthalmologists, angiosurgeons) and even undergo unjustified surgical interventions, which delays the appointment of differentiated therapy.
Over the past 5 years, several cases of FCA have been observed in the neurological departments of the 5th Clinical Hospital in Minsk. When making a diagnosis, frequent diagnostic errors were noted, which prompted their analysis and comparison of our own observations with literature data.
Patient D.
, 68 years old, disabled group II, right-handed, was admitted to the hospital with complaints of visual impairment and decreased memory for current events. He was ill for 4 years, when gradually, for no apparent reason, he noticed difficulty in perceiving visual information. During this period, he could look at an object and sometimes not recognize it, had difficulty recognizing the faces of friends and family members, read text written only in a special font, and began to have difficulty navigating familiar streets, which, in his words, began to “look somehow strange.” Despite visual impairments, he continued to work as a chief designer, but repeatedly consulted an ophthalmologist and was observed for glaucoma, which was excluded by dynamic measurement of intraocular pressure. Subsequently, he was referred to a neurologist for consultation, and Doppler ultrasound of the brachiocephalic arteries was performed, which revealed pathological tortuosity of the internal carotid artery on the left and kinking on the right. The specialists associated the patient’s complaints with these changes and in the angiosurgery department performed a reconstructive operation of resection of the internal carotid artery on the left with elimination of the loop formation (2010), which did not bring improvement. The patient's condition has noticeably worsened over the past year, when, due to visual impairments, he began to move independently with difficulty, decreased memory, the inability to read text in any font, count, and lost 10-20 kg for no apparent reason. He has been examined many times in neurological institutions in our country and in a number of clinics in the USA. Various diagnoses were made: ischemic optic neuropathy, Alzheimer's disease, degenerative disease of the central nervous system. Disability group II has been established. Repeated magnetic resonance imaging (MRI) of the brain excluded ischemic or tumor damage. I took Aricept (donepezil) 5 mg/day and Namenda (memantine) 10 mg/day with some improvement in my condition. Among the previously suffered diseases, he noted rare colds, sometimes increased blood pressure (BP), and benign prostatic hyperplasia. Denied smoking, drinking alcohol or other toxic substances. Higher education, no family history. There were no cases of early dementia in the family: the mother died at the age of 89, the father died young during the Great Patriotic War, two adult sons are healthy. Currently he lives alone, and therefore self-care is significantly difficult.
Objectively upon admission: general condition is satisfactory, low nutrition, blood pressure 130/80 mm Hg, rhythmic pulse 68 beats/min. There is a postoperative scar along the front surface of the neck on the left. No somatic pathology was identified. In consciousness, partially oriented in place and time. Speech is free. The mood is even, behavior is adequate, criticism of one’s condition is somewhat reduced. The memory is weakened, he names the main historical events, but does not remember the age of his youngest son. Serial counting is difficult, he performs multi-step tasks with errors, and is not always able to identify household items by touch (furniture, clothing, keys, etc.). Does not write and cannot read any text. Mini-Mental State Examination (MMSE) score: 16 points (cognitive decline). Performs tests of the frontal dysfunction battery satisfactorily, with the exception of attention tasks when repeating movements, but at the same time he tries to imitate given movements by ear. Associative thinking is impaired: when explaining the main differences between a bird and an airplane, he only names their different wing geometry (an aircraft designer by profession) and the pilot’s control. Cranial nerves: pupils are equal in size, direct and friendly reaction to light is preserved, movements of the eyeballs are complete, distorted color perception (yellow is perceived as red - achromatopsia). The face is symmetrical, the tongue is in the midline, the Marinescu-Radovici reflex is moderately expressed on both sides. Swallowing is not impaired, the soft palate is mobile. The range of motion in the limbs is full, muscle tone is not changed. Tendon-periosteal reflexes are of average vivacity, D=S, there are no pathological foot signs. All types of sensitivity (superficial, deep muscle, two-dimensional-spatial) are preserved. Performs finger-nose and knee-heel tests satisfactorily. The functions of the pelvic organs are not impaired. Walking independently is difficult due to lack of vision control (optical ataxia), but when supported by an accompanying person, the gait is not significantly impaired.
Examination: routine general clinical and biochemical blood tests (including multiple tests for total cholesterol and triglycerides) - without deviations from the norm. In blood serum: vitamin B1 - 59 nmol/l (normal 70-180 nmol/l); vitamin B12 - 440 pg/ml (220-1000 pg/ml); free T4 - 0.9 ng/dl (0.9-1.8 ng/dl); thyroid-stimulating hormone - 1.63 ng/dl (0.35-5.5 ng/dl). ECG: sinus rhythm, horizontal position of the electrical axis of the heart. Ultrasound of the brachiocephalic arteries 6 months after surgery: kinking of the right internal carotid artery with an increase in the linear velocity of blood flow to 128 cm/s, main type; blood flow in the left internal carotid artery is free, the course is straight, moderate hypertonicity in all branches, compression tests are unremarkable. Ultrasound of the heart: atherosclerosis of the aorta and valve structures, systolic function is satisfactory, the chambers of the heart are not dilated. Consultation with a urologist: stage I benign prostatic hyperplasia. Repeatedly examined by an ophthalmologist: visual acuity cannot be checked; When examined with a fundus lens, the optic discs have a grayish tint, there is no edema. Electroretinography: response from both eyes of normal amplitude and shape to all types of stimuli. Tomography of the optic nerve: the structure of the nerve layers in all segments is preserved (Fig. 1).
| Rice. 1. Tomography of the optic nerve of patient D., 68 years old, diagnosed with posterior cortical atrophy: the structure of the nerve layers in all segments is preserved. |
Visual evoked potentials: evidence of bilateral deterioration of visual afferentation to the cortex, more pronounced with stimulation of the left eye. MRI of the brain: expansion of the cortical grooves and ventricles of the brain, expressed in the occipital and parietal lobes, more on the right (Fig. 2).
| Rice. 2. MRI of the brain of the same patient: expansion of the cerebral ventricles and cortical sulci (a), more pronounced in the occipital and parietal lobes on the right (b). |
| ]]> |
| Rice. 2. MRI of the brain of the same patient: expansion of the cerebral ventricles and cortical sulci (a), more pronounced in the occipital and parietal lobes on the right (b). |
| ]]> |
Thus, the patient, aged 64 years, gradually developed visual agnosia, which was initially mistakenly regarded as a pathology of the organ of vision. Subsequently, visual disturbances were explained by chronic cerebrovascular insufficiency in the carotid artery basins due to their kinking and cowling, and even an unsuccessful reconstructive operation was performed. Meanwhile, post factum detected changes should be considered clinically insignificant. Subsequently, after 3 years, cognitive impairment of the cortical type, achromatopsia, acalculia, optical ataxia, apraxia and weight loss were added. Laboratory and instrumental examinations made it possible to exclude pathologies of the eyes, optic nerves, and other somatic or neurological pathologies. A pronounced local bilateral atrophic process, predominant in the parietal and occipital lobes, more on the right, discovered during MRI of the brain, confirmed the diagnosis of posterior cortical atrophy. Combination therapy with cholinergic drugs (dopenesil and akatinol) led to stabilization of the process. A comparison of clinical manifestations, dynamics of the process and examination results in our patient with literature data confirmed their almost complete similarity, with the exception of weight loss, which had not previously been found in the literature.
Posterior cortical atrophy (PCA, Benson's syndrome, visual variant of Alzheimer's disease) as an independent nosological form was first described by F. Benson in 1988 [cit. according to 6]. The author summarized the results of an examination of 5 patients with early development of a complex of visual impairments and progressive dementia.
Subsequently, the mean age of onset was found to be 58 years (range 51 to 64 years). All researchers emphasize the rarity of this pathology. Thus, in a specialized clinic in Lyon in 2001, the share of PCA in the structure of all cases of dementia was only 4% (6 out of 154 new patients with various causes of dementia). The onset of the disease is gradual over several years. The initial manifestations of PCA are visual agnosia and apraxia, which remain the leading symptoms throughout the disease [1, 3].
Visual agnosia is an obligate symptom of PCA, characterized by the inability to identify and identify individual objects or people, despite knowledge of their characteristics, which is associated with damage to the occipital lobes [6, 10]. The complex of visual disturbances in PCA may include elements of Balint's syndrome (optical ataxia, oculomotor apraxia), apperceptive visual agnosia (difficulty in recognizing the features of an object, while its naming is not impaired), alexia, disorientation (patients can get lost in a familiar place), simultaneous agnosia (difficulty in general recognition of an object), prosopagnosia (inability to recognize familiar faces). Unusual visual disturbances in PCA include patients being more fluent in reading small text or unusual font; they see distant objects better than nearby ones [3, 5].
Apraxia in PCA is manifested by difficulties in performing simple and complex movements while maintaining the physical ability to perform them, which is explained by damage to the parietal lobes. Patients with PCA may experience constructive apraxia (the inability to perform a simple configuration or drawing), the inability to dress or undress independently, ideomotor (the inability to perform symbolic gestures) and ideational (impaired creation of a plan for complex movements, use of household appliances or accessories) apraxia. In PCA, Gerstmann's syndrome has been described, which is manifested by agraphia, acalculia, left- or right-sided disorientation, and finger agnosia [1, 5, 6].
Mild cognitive impairment occurs already in the early stages of PCA. Subsequently, they may increase, but never reach the level of severe dementia as in Alzheimer's disease [3]. Speech and motor areas are usually intact. Affective disorders are not observed in patients with PCA, and their behavior resembles that of blind people. The course of the disease is slowly progressive and typically ends in death after 8-12 years, usually from somatic causes, more often from bronchopneumonia [3, 5].
Diagnosis of PCA is based on neurological examination and results of neuropsychological testing. To date, there are no laboratory biomarkers of PCA in serum and cerebrospinal fluid. Neuroophthalmological examination usually does not reveal pathology, but homonymous hemianopsia may be observed. On MRI of the brain, a typical manifestation of PCA is bilateral predominantly parieto-occipital atrophy, more pronounced in the right hemisphere [3]. Unlike Alzheimer's disease, PCA does not show atrophy of the hippocampus and temporal lobes. With single-photon and positron emission tomography, symmetrical areas of hypoperfusion or hypometabolism in the occipital and parietal lobes are typical [3, 5, 6, 10]. Differential diagnosis of PCA is carried out with Creutzfeldt-Jakob disease, tumors or infarctions of the brain in the parietal or occipital localization, and Alzheimer's disease. Treatment of PCA consists of long-term use of cholinergic drugs in an adequate dose and periodic courses of neuroprotectors.
The second observation illustrates the classic course of primary progressive isolated aphasia, in the diagnosis of which diagnostic errors were also observed.
Patient M.
, 66 years old, right-handed, disabled group II (previously worked as an operator), upon admission to the neurological department of the 5th clinical hospital in Minsk, she did not make any complaints due to speech disorders. From the words of relatives and analysis of medical documentation, it was clarified that she had been ill for 3 years, when those around her gradually noticed her “poverty” of speech, difficulty in finding words, and could not always remember the names of objects. The speech disorder slowly increased, which forced the patient to consult a neurologist at the district clinic. Suspected of a cerebral infarction, she was sent for emergency hospitalization to one of the neurological departments in Minsk, where after an examination this diagnosis was confirmed. She was discharged from the hospital with a diagnosis of atherothrombotic cerebral infarction in the left carotid system with moderate motor aphasia, despite the fact that there were no paresis of the limbs, MRI of the brain showed only a diffuse atrophic process, and ultrasound of the great vessels of the head and neck showed only hemodynamically insignificant disorders. Courses of antioxidants, antihypoxants, and nootropics were prescribed—without effect. Speech impairments progressed; therefore, a year later she was hospitalized in the neurological department of another hospital, from where she was discharged with a diagnosis of discirculatory encephalopathy stage II on the background of a cerebral infarction in the left carotid system (no paresis of the limbs was noted in the epicrisis, a repeat MRI also did not reveal any in the brain focal disorders). For this reason, disability group II was established. Speech disorders continued to increase, which forced relatives to go to a third medical institution. Among the previously suffered diseases, she noted calculous cholecystitis, polyosteoarthrosis, and “mild” arterial hypertension (she was inconsistently taking antihypertensive drugs). There is no family history (including dementia).
Objectively upon admission: the patient’s general condition is satisfactory, she has increased nutrition (height 160 cm, body weight 98 kg). Restriction of movement and deformation of both knee joints. Respiratory rate 16/min, blood pressure 130/80 mm Hg, pulse 76 beats/min, rhythmic. No somatic pathology was identified. In consciousness, productive contact is not available. Spontaneous speech is completely absent. Partially understands spoken speech and follows simple instructions. Reading, writing and counting are impaired. The pupils are equal in size, their reaction to light is preserved. The face is symmetrical, slight deviation of the tongue to the right. The strength in the limbs is sufficient, muscle tone is not changed. Tendon-periosteal reflexes are live, D=S, there are no pathological foot signs. Sensitivity cannot be reliably verified. Statics, coordination and gait are not changed. Controls the function of the pelvic organs.
Examination: general clinical blood test - no pathology. In a biochemical blood test, except for an increase in the level of total cholesterol to 6.6 mmol/l, no other abnormalities were detected. ECG: moderate sinus bradycardia, deviation of the electrical axis of the heart to the left. Oculist: it is impossible to check visual acuity; in the fundus, the veins are dilated and the arteries are narrowed. X-ray of the knee joints: pronounced narrowing of the joint spaces, marginal bone growths. Consultation with a speech therapist: severe sensorimotor aphasia. MRI of the brain: diffuse expansion of the ventricular system and cortical sulci, more pronounced in the left hemisphere of the brain. Single photon emission tomography: focus of hypoperfusion in the left frontotemporal region. She received anticholinesterase drugs (neuromidin), pentoxifylline, mildronate without effect. During follow-up, the patient's condition continued to deteriorate. A year later, total aphasia developed, and after 2 years she stopped moving independently, mainly due to apraxia of walking, along with a diffuse increase in muscle tone of the extrapyramidal type, mild right-sided hemiparesis and extensive bedsores. She died at home 6 years later from the first symptoms of the disease; no autopsy was performed.
Thus, a 63-year-old patient gradually developed dysphasia, then isolated motor, and a few years later sensorimotor aphasia, alexia, agraphia and acalculia. These focal symptoms of damage to the higher cortical functions of the dominant hemisphere were initially mistakenly regarded as a cerebral infarction, and then as chronic cerebrovascular insufficiency against the background of residual phenomena after a cerebral infarction in the left carotid system. Meanwhile, the patient had no clinical and instrumental signs of cerebral infarction, and her motor sphere remained completely intact. Only 4 years after the onset of the disease, a diagnosis of primary progressive isolated aphasia was made, confirmed by single-photon emission tomography.
Primary progressive aphasia (PPA) is another clinical form of PCA, the development of which is associated with predominant atrophy in the speech areas of the cortex of the dominant hemisphere while other parts of the brain are intact [1]. With this pathology, patients experience an isolated speech disorder for several years. In the literature [2, 8], PPA is usually divided into three forms depending on the location of atrophy detected on neuroimaging: primary progressive motor aphasia (PPMA), semantic dementia (SD), and logopenic aphasia (LA). PPMA develops with atrophy of the insula and the posterior part of the left frontal lobe, including Broca's area. At the onset, patients’ speech is characterized by agrammatism, difficulty in choosing words and names of objects, slowness, and short phrases. Impressive speech is not impaired. As the process progresses, complete apraxia of speech develops [4, 9]. SD is manifested by a lack of understanding of phrases with complex constructions (father's brother, brother's father), the meaning of prepositions, suffixes, endings, word meanings and speech formulas with spatial relationships. This pathology develops with asymmetric atrophy of the anterior part of the temporal lobe on the left [8]. LA is characterized by a disorder in understanding one's own and others' speech, lack of control, and paraphasia (omissions, substitutions, repetition of sounds or words). The advanced stage of LA is characterized by a “word salad” in the form of an abundance of incomprehensible speech products. The morphological pattern of atrophy in this form is localized in the posterior part of the temporal and lower part of the parietal lobe on the left [2]. After 5-8 years from the onset of the disease, the degenerative process in any form of PPA spreads to the gray and white matter of other parts of the brain, which explains the addition of motor disorders, apraxia and dementia in the clinical picture in these patients [9]. The diagnosis of PPA is confirmed by an asymmetric atrophic process in the frontotemporal region of the dominant hemisphere on MRI and the detection of a hypoperfusion zone there on single-photon emission tomography. A comparison of the clinical manifestations, dynamics of the process and examination results in our patient with literature data confirmed the classic course of PPMA.
Thus, focal cortical atrophies are rare clinical forms of neurodegenerative diseases of the central nervous system, which are distinguished by the selective localization of the atrophic process in individual lobes of the brain and have significant clinical polymorphism. Their etiology and pathogenesis have not yet been fully elucidated. In our opinion, FKA is a neurological syndrome, which, despite its common pathogenesis and pathomorphology, is significantly different from Alzheimer's disease and corticobasal degeneration. Knowledge by practicing doctors of the features of their clinical picture allows them to avoid unnecessary examinations and surgical interventions, timely prescribe differentiated therapy and correctly resolve expert issues.
Treatment and prevention
By following simple rules, it is possible to alleviate symptoms and prolong a person’s life. Once the diagnosis is made, it is advisable for the patient to remain in a familiar environment, since stress aggravates the condition. A person needs feasible mental and physical activity.
A balanced diet is important, you need to restore a clear daily routine. It is necessary to give up bad habits. You also need physical activity and mental exercises. A diet for atrophy involves avoiding heavy, unhealthy foods, you should not eat fast food, and drinking alcohol is strictly prohibited. The menu should include nuts, seafood and greens.
Treatment of brain atrophy involves the use of neurostimulants, tranquilizers, antidepressants and sedatives. This disease cannot be completely cured; therapy can only alleviate the symptoms. The choice of remedy depends on the type of atrophy and the type of impaired functions.
With damage to the cerebellar cortex, treatment is required to restore movement. You also need to use drugs that reduce tremor. Sometimes surgery is needed. Sometimes medications are used that improve metabolism and cerebral circulation, ensuring good blood circulation and protection against oxygen starvation.
Source
The role of a positive attitude
Most experts agree that a calm atmosphere, the right attitude and participation in all daily activities have a positive effect on a person’s well-being. The patient's relatives need to take care that there are no violations of the daily routine.
A positive attitude, active life and lack of stress are the best ways to stop the disease.
The following factors help prevent degenerative phenomena:
- healthy lifestyle;
- healthy eating;
- giving up bad habits;
- constant mental activity;
- blood pressure control.
Treatment of grade 1 cortical atrophy should be timely.