- Causes of pulmonary edema
- What diseases are there a risk of edema?
- Types of pathology
- Symptoms of pulmonary edema
- Diagnostics
- Treatment of pulmonary edema
- Predictions and prevention
Pulmonary edema is a condition in which gas exchange is disrupted and respiratory failure develops. Swelling occurs due to an imbalance of pressure in the pulmonary capillaries and the release of a large amount of edematous fluid into the lung tissue without its reabsorption.
Causes of pulmonary edema
A mixture of edematous fluid (transudate) and a liquid substance that “lines” the alveoli of the lungs from the inside (it is called “pulmonary surfactant”) enters the lumen of the alveoli, where it combines with air. This leads to the formation of foam, which creates an obstacle to the flow of oxygen. Lack of oxygen provokes the development of shortness of breath, due to which the pressure inside the chest decreases and blood flow to the right side of the heart increases.
Pulmonary edema causes infiltration of the alveoli and is manifested by symptoms that indicate oxygen starvation, which is dangerous for tissues. The patient requires emergency care due to the high risk of death due to suffocation.
Questions and answers
What causes pulmonary edema?
There are dozens of factors that contribute to the development of this pathology. They are associated with other diseases of different body systems. Clinical recommendations for pulmonary edema are largely determined by the situation.
Can pulmonary edema lead to death?
Yes, the risk of death in the case of such a pathology is very high, and for the fulminant form it is the only possible outcome of events. This is an extremely dangerous condition that requires immediate professional help.
How to treat pulmonary edema?
This is done exclusively in medical institutions, most often in intensive care. Only doctors know everything you need to know about the symptoms and treatment of pulmonary edema in adults or children - the pathology cannot be eliminated without special knowledge and skills.
What are the features of pulmonary edema in children?
Unlike adults, this pathology occurs much less frequently in children due to other diseases. The underlying cause is usually allergies or exposure to toxins. Or the cause may be congenital anomalies of various body systems.
What diseases are there a risk of edema?
Pathology indicates a complication of the underlying disease, increases its duration and worsens the prognosis of treatment. The most dangerous from the point of view of pulmonary edema include:
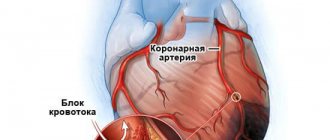
- Heart diseases. Respiratory failure often occurs against the background of pathologies of the heart and blood vessels. Cardiogenic pulmonary edema is a life-threatening complication that develops with myocardial infarction, aneurysm, endocarditis and myocarditis, severe hypertension, and pathological conditions caused by congenital or acquired heart defects.
- Pulmonary diseases. At risk are patients with injuries and severe diseases of the respiratory tract. Respiratory edema develops against the background of exacerbation of chronic bronchitis and bronchial asthma, tuberculosis, and lobar pneumonia. The risk is increased by tumor lesions of the lung tissue, pleurisy, and chest injuries, which are accompanied by pneumothorax. If a person is connected to a ventilator for a long time and receives a mixture with a high concentration of oxygen, this also leads to an imbalance of pressure in the pulmonary capillaries and the release of exudate.
- Infectious diseases. In severe cases or inadequate treatment of whooping cough, scarlet fever, influenza, diphtheria and other infectious diseases, edema develops, followed by acute pulmonary failure. In young children, this clinical syndrome can cause acute laryngitis and the proliferation of adenoids.
- Pathologies of intrauterine development and difficult childbirth. Severe pregnancy, prematurity, oxygen hypoxia, fetal bronchopulmonary dysplasia - these factors increase the risk of developing pulmonary failure in newborns. In pregnant women, pulmonary failure can develop due to eclampsia. The same phenomenon occurs with ovarian hyperstimulation syndrome against the background of stimulation of ovulation by hormonal drugs.
- Foreign bodies entering the respiratory tract. Mechanical asphyxia is one of the possible causes of acute respiratory failure. Pathology occurs when foreign objects enter the respiratory tract, after drowning or attempted hanging, or blockage of the respiratory tract with vomit.
- Diseases of the urinary system and gastrointestinal tract. Nephrogenic pulmonary edema can be complicated by acute inflammatory diseases, which are accompanied by renal dysfunction and the development of severe renal failure. In gastroenterology, patients with liver cirrhosis, severe pancreatitis, and intestinal obstruction have to deal with respiratory failure.
- Neurological diseases. Traumatic brain injuries, meningitis, encephalitis, neoplasms, cerebral hemorrhages, complications after brain surgery - all this leads to neurogenic pulmonary edema.
- Allergies, injuries, poisoning. Acute respiratory failure can be caused by the ingestion of various toxic substances into the body. Pulmonary edema is encountered by patients with alcohol and drug intoxication, poisoning with drugs, salts of heavy metals, and toxic gases. Pulmonary insufficiency is diagnosed in case of blood poisoning, burns with a large affected area, acute allergic reactions.
Cardiogenic form
Cardiogenic OB occurs as a manifestation of left ventricular heart failure. The following diseases can lead to the development of pathology:
- myocardial infarction, post-infarction conditions;
- acquired heart defects (both aortic and mitral);
- hypertensive crisis;
- disturbances of heart rhythm and conduction (arrhythmias, blockades).
The mechanism of development of the cardiogenic form of edema is associated with an increase in pressure in the pulmonary capillaries. This occurs due to increased diastolic pressure in the left ventricle.
The left ventricle cannot contract enough to push all the blood out of the cavity into the aorta. This leads to an increase in pressure first in the left ventricle and then in the left atrium. Since the pulmonary veins flow into the left atrium, over time the pressure also increases in the pulmonary circulation. The fluid sweats first into the interstitial tissue and then into the alveoli.
By the same principle, the lungs swell due to hypervolemia (increased blood volume).
Hypervolemia can develop as a complication of infusion therapy.
Types of pathology
Depending on the cause of development, pulmonary edema can be cardiogenic or non-cardiogenic. In the first case, the cause of respiratory failure is cardiovascular disease. The second category includes all other pulmonary edema caused by diseases of the gastrointestinal tract, nervous system, and injuries.
Pulmonary edema is also classified according to the nature of its course. There are four types of pathology development:
- With fulminant development, severe respiratory failure occurs within a few minutes and leaves no chance of survival.
- Acute swelling can take up to four hours to develop. This form is considered less dangerous than the previous one, but in the absence of timely assistance, the risk of death is extremely high. Most often, acute pulmonary edema develops with myocardial infarction, traumatic brain injury, and acute allergic reactions.
- In case of intoxication, renal and liver failure, subacute pulmonary edema may occur. The intensity of symptoms is constantly changing, so continuous medical monitoring of the patient's condition is required.
- Prolonged swelling may take several days to develop. Symptoms are mild compared to the acute and subacute forms. Prolonged pulmonary edema usually occurs against the background of various chronic diseases, including heart failure.
Symptoms
It is possible to describe the symptoms of pulmonary edema only in general terms, since certain types of pathology occur with blurred characteristics. Signs include the following:
- severe weakness;
- shallow, very rapid breathing;
- dry cough;
- dry wheezing;
- severe shortness of breath;
- puffiness of the face and neck;
- bubbling breathing and moist wheezing;
- foam at the mouth with a pink tint;
- lethargy, confusion;
- shallow breathing;
- thready pulse.
Some signs of pulmonary edema contradict each other for the reason that everything can start with one condition and end with another. For example, rapid breathing occurs for several minutes or hours, and then it weakens. In the fastest and most dangerous forms of edema, the patient's death occurs from suffocation (asphyxia).
Are you experiencing symptoms of pulmonary edema?
Only a doctor can accurately diagnose the disease. Don't delay your consultation - call
Symptoms of pulmonary edema
Before the main symptoms of pulmonary failure appear, patients experience weakness and dizziness, a feeling of tightness in the chest, headache, and dry cough. A few hours after the first symptoms of the pathology, an attack of cardiac asthma develops - the first stage of pulmonary edema. It manifests itself:
- severe lack of air;
- severe dry cough;
- increased heart rate;
- hoarse breathing;
- profuse sweating;
- pale skin, blueness of nails and lips;
- feelings of fear and anxiety.
As a rule, the attack occurs at night or before dawn. In patients with cardiac diseases, cardiac asthma can be caused by physical or emotional stress and hypothermia.
As edema develops, the alveoli become involved in the pathological process. This leads to increased suffocation. The patient experiences severe shortness of breath, the face becomes burgundy-blue and puffy, the veins in the neck swell, and mental retardation appears. Breathing becomes hoarse, foam mixed with blood comes out of the mouth.
In the absence of medical care, the patient loses consciousness and falls into a coma. In this state, blood pressure decreases critically, breathing becomes shallow, and the pulse weakens. The cause of human death is asphyxia, in which the body experiences an acute lack of oxygen with an excess of carbon dioxide.
Consequences for life
The prognosis depends on several factors: timeliness of care, concomitant pathology and severity of the condition. The danger of the disease is the development of acute respiratory failure. Because of this, not only the respiratory system suffers, but also all organs that do not receive enough oxygen.
In many cases the prognosis is poor. Old age is one of the risk factors that aggravates the course of the disease.
With OL, patients die from asphyxia. With early treatment (at the stage of interstitial edema), complete recovery is possible. The prognosis largely depends on the cause; with cardiogenic shock or sepsis, the mortality rate is several times higher.
Diagnostics
A doctor can determine the development of pulmonary edema by numerous external symptoms. In addition, the patient is prescribed instrumental and laboratory examinations. Among them:
- measurement of blood oxygen levels, determination of carbon dioxide content;
- blood chemistry;
- electrocardiogram and ultrasound of the heart;
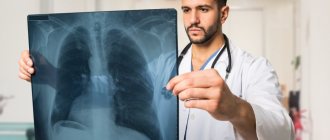
- chest x-ray to evaluate the condition of the lungs.
Inserting a catheter into the pulmonary artery allows you to determine the type of edema: cardiogenic or non-cardiogenic.
If pulmonary edema is suspected, it is important to carry out the necessary tests and examinations as soon as possible, identify the cause and type of pathology, and begin treatment. Saving the patient's life directly depends on this.
Hospital treatment
Treatment of the pathology is carried out in a hospital setting and includes the following measures: oxygen therapy, the prescription of diuretics and cardiac glycosides, intravenous administration of albumin, heparin, atropine, aminophylline. In some cases, hormones are prescribed. All prescriptions are strictly individual and are adjusted taking into account the patient’s condition.
The prognosis for treatment of cardiogenic pulmonary edema depends on the type of pathology, severity, presence of concomitant diseases, as well as the quality of medical care provided.
Treatment of pulmonary edema
People with acute respiratory failure are treated in the intensive care unit. First aid consists of measures that reduce venous return to the heart. To do this, the patient must take a semi-sitting position. Applying tourniquets to the limbs and hot foot baths have a positive effect.
It is imperative to monitor blood oxygen saturation levels. Oxygen therapy is used to compensate for its deficiency. If pulmonary edema has developed against the background of mechanical asphyxia, it is necessary to clear the airways of foreign objects. If it is impossible to breathe independently, the patient is connected to a ventilator.
A combination of medications is used to eliminate pulmonary edema. Among them:
- morphine and other narcotic analgesics;
- drugs to stimulate diuresis;
- nitroglycerine;
- drugs to lower blood pressure.
Depending on the underlying disease, patients with pulmonary edema are prescribed antihistamines, antibiotics, hormonal and antiarrhythmic drugs, and cardiac glycosides. The task of the resuscitator is to stop the attack and prevent acute hypoxia, which leads to cell death and death of the patient. After the symptoms of respiratory failure are relieved, treatment of the disease that caused it begins.
It is very important to eliminate the root cause that led to the clinical syndrome. Otherwise, a relapse of the disease is possible.
Treatment
Treatment includes several areas - emergency measures at the prehospital stage, oxygen inhalation, drug therapy in the hospital. Treatment tactics depend on the form of the disease - cardiogenic or non-cardiogenic.
Treating pulmonary edema at home, using improvised means, is strictly contraindicated. It is necessary to provide qualified medical care.
How to help a sick person at home
Pulmonary edema is a medical emergency that requires immediate medical attention. First aid can be provided at home before the ambulance arrives. How to alleviate the condition:
- Place the person in a sitting position with their legs down.
- Provide access to fresh air - open a window, ventilate the room.
- Unfasten clothing if it is constricting your neck and chest.
- Hot foot baths. They increase blood flow to the legs, reducing the return to the pulmonary circulation.
- If possible, tourniquets or cuffs may be applied to the limbs. This will slow down the development of symptoms.
After the ambulance arrives, you must follow the instructions of the medical personnel. Further treatment includes taking medications, which are prescribed by a doctor depending on the cause and severity of the condition.
If symptoms of pulmonary edema appear, emergency medical attention is required
Basic treatment
Drug therapy for OA in older people includes the use of general and etiotropic drugs. Basic treatment includes the use of the following medications:
| Nitrates | They reduce pressure in the pulmonary capillaries, this reduces congestion in the pulmonary circulation and, accordingly, swelling. In addition, they reduce the load on the heart, which is necessary for cardiogenic edema. Nitrates include Nitroglycerin (a short-acting drug that must be administered every 3-5 minutes) and Sodium Nitroprusside (a longer-acting drug, 20-30 minutes). |
| Painkillers | Narcotic analgesics, usually morphine, are used to reduce pain. Morphine not only reduces pain, but also eliminates the influence of the sympathetic nervous system (vasospasm). |
| Diuretics | Loop diuretics are usually used - Furosemide, Torsemide. Their effect occurs quickly, within 5–7 minutes. Reduced swelling is associated not only with increased fluid removal, but also with dilation of the veins. |
Elderly people have many concomitant diseases, which makes it difficult to select treatment. For example, nitrates are contraindicated for the treatment of patients with mitral or aortic stenosis, arterial hypotension, and severe tachycardia.
When prescribing drug therapy, it is imperative to determine the cause of edema and concomitant pathology.
In case of OA, treatment is also aimed at improving blood oxygenation, using respiratory support. The patient is given oxygen through a face mask or nasal cannulas. Use breathing mixtures with a high oxygen content - 60–100%. Oxygen is supplied through defoamers, for example, ethyl alcohol.
Treatment depending on the cause
For OL, treatment is also used to get rid of the cause:
- For cardiogenic shock , drugs are used that increase myocardial contractility and vascular tone. The first group includes cardiac glycosides (Korglykon), the second - Dopamine, Dobutamine, Levosimendan.
- In case of heart rhythm disturbances, antiarrhythmic drugs are used, for example, Amiodarone, Lidocaine.
- For pneumonia, antibacterial agents are prescribed.
- In case of hypertensive crisis, drugs that lower blood pressure are additionally prescribed - beta blockers, ACE inhibitors.
Predictions and prevention
Pulmonary edema is a deadly condition; Mortality with this clinical syndrome is up to 50%. Patients with anaphylactic shock most often develop fulminant or acute pulmonary edema, which in more than 90% leads to death.
The consequences of acute pulmonary failure are no less serious than the disease itself. Many patients who have suffered pulmonary edema experience ischemic damage to internal organs, the appearance of areas of pneumosclerosis, and congestive pneumonia. This affects the functioning of the respiratory system, in the organs of which irreversible changes occur. The pathology is manifested by shortness of breath, chest pain, and cough. Pneumosclerosis and other consequences of pulmonary edema require long-term treatment, can lead to disability and shorten the patient's life expectancy.
The likelihood of a favorable prognosis and outcome of the disease with pulmonary edema increases if the diagnosis was made in a timely manner and doctors began to stop the attack at the initial stage.
Non-cardiogenic form
Toxic OA is more common in older people than in other age categories. Non-cardiogenic edema is caused by damage to the blood-air barrier. As a result, there is a violation of the permeability of fluid into the interstitial space and alveoli. This is possible under the following conditions:
- respiratory tract burn;
- pneumonia;
- chest injury;
- septic conditions;
- pancreatitis;
- renal failure;
- acute cerebrovascular accident;
- poisoning with drugs (for example, salicylates);
- poisoning with toxic substances.
The mechanism of development of pulmonary edema in these conditions is associated with the action of toxins (poisons, bacterial exotoxins, metabolites in renal failure, etc.) on the endothelium of the pulmonary capillaries.
Causes
Cardiogenic pulmonary edema is caused by heart disease in the decompensation stage. In addition to such common phenomena as myocardial infarction, arrhythmias, heart defects, the following conditions can cause pathology:
- cardiomyopathy;
- atrial tumor;
- endocarditis of bacterial origin;
- inflammatory process of the aorta;
- myocarditis;
- mitral valve stenosis;
- acute failure of the left ventricle of the heart;
- cardiosclerosis.
If cardiovascular diseases have not been treated, the development of cardiogenic pulmonary edema is possible with any pathology. Various intrauterine developmental disorders can provoke severe complications, for example, ventricular septal defect, coarctation of the aorta, patent ductus arteriosus.
Cardiogenic pulmonary edema always develops against the background of cardiac pathologies
Predisposing factors include bad habits, frequent emotional overload, increased blood pressure, lack of treatment for heart pathologies, non-compliance with doctor's orders, and more.
Pre-hospital emergency care
- At the first signs of pulmonary edema, the patient or those around him should call an ambulance.
- Place the patient in a semi-sitting or sitting position with legs down.
- Ensure a sufficient flow of fresh air, open windows and vents, and remove clothing that restricts breathing from the patient.
- Constantly monitor your breathing and pulse.
- Measure (if possible) blood pressure.
- Place the patient's feet in hot water.
- Apply a tourniquet to the thigh for 30-50 minutes, then apply it to the other thigh.
- Inhale alcohol vapor (for adults 96%, for children 30%).
- At a pressure of at least 90 mm. Hg Art. Give the patient a Nitroglycerin tablet under the tongue.
- Give the patient a Furosemide (Lasix) tablet.
Prevention measures
Eliminating the causes that can provoke pulmonary edema is the prevention of the disease. To prevent a dangerous condition, you must adhere to the following rules:
- eat healthy and nutritious food. The diet should contain a large amount of minerals, vitamins and other nutrients. It is important to avoid foods that increase blood cholesterol;
- Each person is recommended to exercise and often walk in the fresh air;
- give up cigarettes, drugs and alcohol;
- promptly treat cardiovascular pathologies;
- avoid conflicts and stressful situations;
- normalize body weight;
- When working with harmful substances, you must strictly follow safety rules.
It should be remembered that it is impossible to completely insure against the development of pulmonary edema. The condition occurs suddenly, sometimes the patient is not even aware of problems with the heart or other organs. Compliance with prevention and a healthy lifestyle will help to significantly reduce the risk of a dangerous pathology. Timely assistance to a patient with developed pulmonary edema significantly increases the patient's chances of survival.