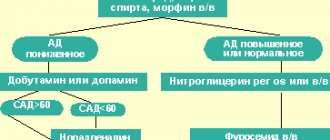
Pathophysiology of oxidative stress
The basic mechanisms of pathology in any critical condition, including surgical and traumatic aggression, are free radical processes and changes in the properties of cell biomembranes. The main pathological role of free radicals is that they actively interact with molecules that form neuronal and intracellular membranes. The viscosity of the membranes increases, their plasticity and functional state are lost. Along with this, genes responsible for programmed cell death - apoptosis - are activated. There is a direct relationship between the accumulation of lipid peroxidation products and the severity of damage to nerve cells and other tissues.
Since the formation of tissue hypoxia, lipid peroxidation, and mitochondrial dysfunction are recognized as the trigger for the development of a typical pathological process, the use of antihypoxants and antioxidants is pathogenetically justified in surgical and traumatic aggression, inflammation and acute pain.
Restoring blood flow in previously ischemic tissues also poses a certain danger. Reperfusion causes a multiple increase in the partial pressure of oxygen with a further increase in free radical processes. In this case, the endothelium of the capillaries is damaged, the anticoagulant activity of which is transformed into procoagulant activity. Due to increasing adhesion, leukocytes and platelets clog the capillaries. This process is aggravated by an increase in the rigidity of red blood cells, which sharply increases the disruption of oxygenation of tissues, especially the brain. The processes of blood fibrinolysis are inhibited, the area of cerebral infarction expands, and cerebral edema increases.
The main pathological processes initiated by excessive activation of LPO
I. Cellular-tissue level:
- ischemia;
- hypoxia;
- membranopathy:
– disruption of the permeability of the cell membrane and membranes of cell organelles;
– excessive accumulation of free radicals inside the cell;
– release of lysosomal enzymes into the cell;
– accumulation of Ca++ ions inside the cell;
- apaptosis and cell necrosis;
- violation of cellular reception;
- energy and metabolic disorders.
II.
Organs and systems:
- functional disorders;
- organic pathology.
Of course, the body has an endogenous antioxidant system (AOS), but at critical levels of hypoxia and LPO it is untenable and it is necessary to introduce antioxidants from the outside.
Disorders of energy and metabolic processes in cells and tissues
Reasons for initiation (strengthening) gender
- stress;
- ischemia;
- hypoxia;
- tissue reperfusion; (reperfusion syndrome);
- inflammation (aseptic or bacterial);
- insufficient activity of the physiological antioxidant system (relative and absolute).
If patients' own AOS is insufficient, it is necessary to administer antioxidants and antihypoxants as quickly as possible. Only a few of them are used clinically. Reambirin is used quite widely in anesthesiological and surgical practice as an infusion and energy preparation of a polyonic composition, which contains sodium succinate.
Reamberin:
- 1.5% infusion solution:
- Sodium chloride – 6.0 g
- Potassium chloride – 0.3 g
- Magnesium chloride – 0.12 g
- N-(1-deoxy-D-glucitol – 1-
- N-methylammonium sodium succinate – 15 g
- Water for injections – up to 1 l
However, its antioxidant properties for the correction of oxidative stress in surgical practice and in acute pain have not been studied enough. In the anesthetic aspect, the domestic drug Mexidol from the group of synthetic antioxidants and antihypoxants is currently interesting.
Mexidol
- international proprietary name – hydroxymethylethylpyridine succinate
- chemical rational name – 3-hydroxy-6-methyl-2-ethylpyridine succinate
- dosage form: solution for injection 5% in ampoules of 2 ml n 10. One ampoule with 2 ml solution for injection contains 100 mg of the active substance. tablets 125 mg n 30.
- According to the chemical structure, Mexidol is a salt of succinic acid (succinate).
According to available information, Mexidol is an antioxidant, a free radical inhibitor, a membrane protector, reduces the activation of lipid peroxidation, and increases the activity of the physiological antioxidant system as a whole.
Pharmacokinetics of Mexidol
Has high bioavailability. It dissolves well in water. It has high lipophilicity. It quickly passes from the bloodstream into organs and tissues and is quickly eliminated from the body. High lipophilicity and its ability to bind to blood plasma proteins and endoplasmic reticulum membranes suggest the possibility of the formation of its tissue and blood depot.
Due to the presence of a 3-hydroxypyridine derivative in its composition, which is an active carrier, it penetrates into the cell and mitochondria
(Dumaev K.N., 1995).
The maximum concentration at doses of 400-500 mg is 3.5-4.0 mcg/ml. The retention time (MRT) of the drug in the body is 0.7-1.3 hours.
When administered intramuscularly
– the time to reach maximum concentration is 0.45-0.50 hours.
– determined in blood plasma for 4 hours after administration.
the time to reach maximum concentration (Tmax) in blood plasma is 0.46-0.50 hours;
– the half-elimination period (T1/2 et) and the average retention time (MRT) of the drug in the body are 4.7-5.0 hours and 4.9-5.2 hours, respectively.
Intensively metabolized in the liver with the formation of its glucuron-conjugated metabolites. It is excreted by the kidneys mainly in the form of glucurone-conjugated metabolites. On average, over 12 hours, 0.3% of the unchanged drug and 50% in the form of glucuronoconjugate are excreted in the urine.
Toxicology:
- Acute toxicity
– with oral administration LD50 = 4 g/kg body weight, with intravenous administration LD50 = 800 mg/kg body weight. Therapeutic index ND50 /ED50 =6.2, and LD50 /ED50 =16.4 or more - Chronic toxicity
: with long-term use orally and parenterally in experimental animals, no significant changes in organs and tissues were detected.
Contraindications:
- hypersensitivity;
- acute disorders of liver and kidney function
- childhood, pregnancy, breastfeeding (since no clinical trials have been conducted).
Side effects
(extremely rare):
- drowsiness;
- dry mouth.
Side effects (drowsiness, potentiation of other anesthetics, dry mouth can be successfully used in patients as premedication before surgery. After all, we usually deliberately use relanium and atropine for these purposes.
3-hydroxypyridine derivatives
(included in Mexidol)
They play a big role in metabolism.
- Necessary for the normal functioning of the central nervous system.
- They are part of enzymes that carry out decarboxylation and transamination of amino acids.
- Participate in the metabolism of tryptophan, methionine, cysteine, glutamic and other amino acids, histamine.
- Participate in lipid metabolism processes, improving lipid metabolism in atherosclerosis.
Features of the Krebs cycle reaction associated with succinate
Features of the Krebs cycle reaction associated with succinate:
- Oxidation of succinate is a prerequisite for the catalytic effect of the intermediate on the uptake of oxygen by the cell
- To replenish the pool of organic acids, it is enough to introduce one succinate
- The activity of succinate dehydrogenase does not depend on the concentration of NAD and NADH
- The power of an energy production system using nuclear fuel is hundreds of times greater than all other systems
- The phenomenon of rapid oxidation of succinate in the cytoplasm of cells with reduction of dinucleotide
Activation of oxidative stress during surgery and anesthesia is a key link in the development of pathophysiological processes of critical conditions. And the level of oxidative stress is a modern criterion for the adequacy of anesthesia. There is no doubt about the need to include antioxidants and antihypoxants in anesthesia in order to improve the protection of the operated patient from surgical aggression. At the same time, this issue has been practically not studied.
In our clinic, together with the Department of General Surgery (Head Prof. Yu.S. Vinnik), oxidative stress in surgical patients and the possibility of its correction with antioxidants and neuropeptides have been studied for a number of years. In particular, oxidative stress during operations on the biliary tract was studied.
Go to the contents of the book “Pacifying Pain”
Antioxidants in the treatment of cerebrovascular diseases
Currently, cerebrovascular pathology ranks second among the main causes of mortality, second only to heart disease and already ahead of mortality from tumors of all locations. Cerebrovascular pathology is the leading cause of disability in the population and, therefore, represents one of the most important medical and social problems.
Today, about 9 million people worldwide suffer from cerebrovascular diseases. The leading role among these diseases is occupied by strokes, affecting from 5.6 to 6.6 million people annually and claiming 4.6 million lives. According to the World Health Organization, the incidence of stroke ranges from 1.5 to 7.4 per 1000 people. Thus, in the United States, a cerebral stroke occurs every 53 seconds.
In the Russian Federation and CIS countries, there is a progressive increase in the incidence of this pathology: approximately every 1.5 minutes, one of the Russians develops a stroke for the first time. The incidence of stroke in Russia is 450,000 cases per year: in Moscow alone, the number of acute strokes ranges from 100 to 120 cases per day. The overall mortality rate from stroke in 2001 was 1.28 per 1000 people (men - 1.15, women - 1.38). The mortality rate from stroke in our country is one of the highest in the world: in 2000, the standardized rate was 319.8 per 100,000 people. In terms of mortality rates, Russia ranks second, second only to Bulgaria. Mortality in the acute stage of all types of stroke is approximately 35%, increasing by another 12–15% by the end of the first year. Along with high mortality, the consequences of strokes are also socially significant - the development of disability with loss of ability to work. Disability after a stroke ranks first among all causes of primary disability, since less than 20% of survivors return to their previous social and work activities. In addition, enormous damage is caused to the economy, taking into account the costs of treatment, medical rehabilitation, and losses in production. In the USA, material costs for strokes range from 7.5 to 11.2 million dollars per year, costs per patient, taking into account the need for long-term treatment and social rehabilitation, range from 55 to 73 thousand dollars per year.
The ratio between ischemic and hemorrhagic stroke was previously 5:1. Registry data from 2001 showed that in Russia ischemic strokes amounted to 79.8%, intracerebral hemorrhages - 16.8%, subarachnoid hemorrhages - 3.4%.
In Russia, up to 100,000 new cases of cerebral hemorrhages are registered annually. The incidence of hemorrhagic stroke is higher in men, while the mortality rate is higher in women. According to a number of authors, mortality from cerebral hemorrhage varies from 38 to 93%, with 15–35% of patients dying within a month from the moment of illness, half of them die within the first three days. Only 10% of patients by the end of the first month and 20% after six months can care for themselves; 25–40% of patients have a moderate degree of disability, 35–55% have severe disability.
The epidemiological and demographic situation in the world regarding cerebrovascular pathology is currently characterized by the widespread prevalence of this type of pathology, the “aging” of the population and the increase in the frequency of progressive cerebrovascular diseases, the “rejuvenation” of strokes due to the increase in the number of extreme factors and impacts (A. A. Mikhailenko and co-authors, 1996; A. A. Skoromets, 1999). In a large number of people over the age of 50, the processes of so-called “normal aging” are quickly replaced by pathological changes associated primarily with insufficiency of cerebral blood flow due to atherosclerotic damage to the vessels supplying blood to the brain, with changes in the rheological properties of the blood, leading to dysregulation and decreased neurotransmitter activity. Clinically, these neurotransmitter and morphological dysregulations are manifested by severe symptom complexes of acute and/or chronic cerebral ischemia, requiring constant and effective correction.
The number of patients with symptoms of chronic cerebral ischemia in our country is growing as steadily as the number of patients with acute cerebrovascular accidents, amounting to at least 700 per 100,000 people. While our country currently has statistics on acute strokes, albeit not in full, there are no reliable statistics on the number of patients with chronic cerebral ischemia. These are mainly outpatient patients; visiting a clinic is often difficult for them; Often they are given complex diagnoses, while cerebrovascular pathology is not taken into account or is classified as a complication, which makes it difficult to obtain objective data. The shortage of qualified neurologists in outpatient clinics also often leads to incorrect interpretation of this diagnosis.
Pathomorphological disorders in patients with acute and chronic cerebral ischemia are based on a variety of pathogenetic factors, such as atherosclerosis, arterial hypertension, as well as their combinations, cardiac pathology, changes in the condition of the spine with compression of the vertebral arteries, hormonal disorders leading to changes in the coagulation system blood, other types of disorders of the hemostatic system and physicochemical properties of blood, leading to the formation of functional and morphological ischemic disorders.
The most common causes of the formation of clinical manifestations of cerebral ischemia are atherosclerotic stenotic and occlusive lesions of the main arteries of the head; heart diseases, which include primarily coronary heart disease with symptoms of atrial fibrillation and a high risk of microembolization into intracerebral vessels. Atherosclerosis is a systemic vascular disease that leads to infiltration of the intima of the arteries with cholesterol coming from the blood. In the development of atherosclerosis, hereditary predisposition and constitutional characteristics play a role. However, the main reason for the wide spread of atherosclerosis in recent years is the functional effects on higher nervous activity of a person, which can be classified as negative manifestations of urbanization in the conditions of scientific and technological progress. They lead to long-term and systematic neuropsychic stress. The development of atherosclerosis is promoted by physical inactivity and hypokinesia (work without physical exertion, limited walking, passive rest), hypoxia (urban air pollution), increased exposure to external electromagnetic potential, the negative impact of noise and the pace of city life, insufficient sleep and excess calorie content of food (taking into account hypokinesia). The widespread use of smoking in recent years as a factor contributing to the development of vasospasms in various vascular systems is also of known importance. In this regard, in recent years, about a contingent of patients with atherosclerosis and arterial hypertension, in particular, from 50 to 60% of cases of cerebral vascular diseases occur between the ages of 50 and 60 years. At the same time, cerebral atherosclerosis takes first place compared to arterial hypertension. Four of the factors noted above are of leading importance in the development of vascular cerebral pathology, in particular atherosclerosis: neuropsychic stress, hypokinesia, physical inactivity and excess calorie intake. As a result of their influence, overexcitation of the cerebral cortex and the hypothalamic-pituitary-adrenal system occurs, increased release of catecholamines, disruption of all types of metabolism, especially in the walls of blood vessels, and sometimes increased blood pressure.
The study of the causes of morbidity and mortality in vascular diseases of the nervous system has led to the establishment of risk factors that play a contributing role in the development of cerebral vascular accidents. These factors include: arterial hypertension, vascular hypotension, obesity (overweight), hypercholesterolemia (especially in young and middle-aged people), smoking, alcohol abuse, family history, coronary atherosclerosis, diabetes mellitus, endocrine pathology, mineral metabolism disorders (cervical osteochondrosis), living in areas with sharp fluctuations in meteorological factors, work with high intellectual stress.
Hemorrhagic stroke, also characterized by a severe secondary ischemic cascade, most often occurs as a complication of arterial hypertension (60% of cases). The development of degenerative changes (lipohyalinosis, fibrinoid necrosis) in small perforating arteries of the brain and the formation of microaneurysms against the background of arterial hypertension are the most important prerequisites for the occurrence of hypertensive intracerebral hemorrhage, and hemorrhage develops more often in patients with severe or moderate arterial hypertension than in patients with “mild” » arterial hypertension. Pathogenetically, intracerebral hemorrhages develop due to rupture of a vessel or through diapedesis. The next most common etiological factor for cerebral hemorrhage is rupture of an arteriovenous malformation, hemorrhage from ruptured aneurysms (10–12% of cases). Occurring more often in old age, cerebral amyloid angiopathy, which is formed due to the deposition of abnormal amyloid protein in the tunica media and adventitia of small cortical arteries and arterioles, contributes to the occurrence of miliary aneurysms and fibrinoid necrosis of the affected vessels, which can rupture when blood pressure rises, causing intracerebral hemorrhage in 10 % of cases. Such hematomas are often multiple. Long-term use of anticoagulants in 8–10% of cases leads to intracerebral hemorrhage, especially when hypocoagulation is achieved, i.e., a decrease in the prothrombin index to 40% or an increase in the international normalizing coefficient to 5. Brain tumors or brain metastases are complicated by hemorrhages in them in 6 -8% of cases. Up to 20% are other causes, such as hemophilia, thrombocytopenia, leukemia, hemorrhagic diathesis, arteritis, thrombosis of intracranial veins, alcohol and drug abuse, coagulopathy, vasculitis.
The mechanism of development of hypoxia, which is a discrepancy between tissue demand for oxygen and its delivery, is the same for any form of cerebrovascular pathology. It is associated primarily with impaired oxidation of substrates in body tissues as a result of difficulty or blockade of electron transport in the mitochondrial respiratory chain, which leads to damage to lysosome membranes with the release of utilitarian enzymes into the intercellular space.
Stress, or more precisely distress according to Selye’s theory, is a mechanism of nonspecific adaptation to the changing conditions of the organism’s environment.
At the initial stage of oxygen starvation in mitochondria, the rate of aerobic oxidation and oxidative phosphorylation decreases, which leads to a decrease in protein synthesis and gene expression, a decrease in the amount of adenosine triphosphate (ATP), an increase in adenosine diphosphate (ADP) and adenosine monophosphate (AMP); the ATP/ADP+AMP ratio decreases. With a further decrease in cerebral blood flow, the enzyme phosphofructokinase (PFK) is activated, anaerobic glycolysis is enhanced, and then a final transition to anaerobic respiration is noted, which adapts the cell to hypoxia, but glycogen reserves are depleted. This, in turn, entails the accumulation of under-oxidized lactate, a decrease in pyruvate with the development of lactic acidosis - up to the development of cerebral edema.
At the same time, the activity of lactate dehydrogenase increases and the activity of succinate dehydrogenase, which supplies electrons to the respiratory chain of mitochondria, decreases, which indicates a disruption in the processes of energy formation in the ischemic brain. Under such conditions, anaerobic glycolysis does not occur, which leads to severe energy deficiency. At the final level, destabilization of cell membranes occurs, disruption of the functioning of ion channels, damage to the potassium-sodium pump, potassium (an excitatory neurotransmitter) leaves the cell, which makes it less excitable, and sodium enters the cell in excess, followed by sodium along the osmotic gradient and enters the cell Excessive amounts of water leaving the interstitium accumulate, which leads to cell hyperhydration, cloudy swelling, and then balloon degeneration. The most important role in this process belongs to glutamate receptors.
Oxidative stress, closely associated with the ischemic cascade, occurs when glutamate receptors are excited and consists of excessive accumulation of free radicals, activation of lipid peroxidation and excessive intracellular accumulation of their products. The reactions of oxidative stress and the ischemic cascade interact and potentiate each other.
Free radicals (these are molecules with an unpaired electron) are highly reactive forms of oxygen, hydrogen peroxide, aldehydes formed under hypoxic conditions, with incomplete reduction of oxygen, changing the functional properties of a number of enzymes, carbohydrates, proteins, including deoxyribonucleic acid (DNA) and ribonucleic acid (RNA), as a result the cell loses its functions, abnormal proteins appear and, in addition to the direct damaging effect, secondary destructive processes are stimulated. Oxygen for any cell, especially for a neuron, is the main energy acceptor in the mitochondrial respiratory chain. By binding to the iron atom of cytochrome oxidase, the oxygen molecule undergoes four-electron reduction to form water. The main stable form of oxygen is “triplet” oxygen, in the molecule of which both unpaired electrons are parallel and their valences (spins) are directed in the same direction. Oxygen, in the molecule of which the valences are directed in different directions, is called singlet, it is unstable and toxic for biological substances. Free radicals are unstable and tend to transform into stable compounds by pairing a free radical, tearing off an atom, most often hydrogen, from another compound and attaching it to itself.
Along with the processes of free radical oxidation, stable antioxidant radicals are produced in biological objects, which are capable of abstracting hydrogen atoms only from special molecules that have weakly bound hydrogen atoms. This class of chemical compounds is called antioxidants, since their mechanism of action is based on inhibition of free radical processes in tissues, which inhibits the development of destructive changes and inactivates oxidative stress reactions. Changes in the structure and function of substrates under conditions of ischemia and stress depend on the ratio of the activity of free radicals and antioxidants.
It should be noted that the pathophysiological mechanisms of the emergence and progression of oxidative stress in patients with any form of cerebrovascular pathology are the same and are characteristic of both patients with ischemic and hemorrhagic stroke and patients with chronic forms of cerebrovascular insufficiency. Chronic cerebral ischemia is a disease that progresses stepwise against the background of repeated episodes of dyscirculation, leading to an increase in brain hypoxia.
Treatment of cerebral stroke consists of general and specific methods. The first include measures to ensure adequate oxygenation, correction of blood pressure, relief of complications, possible seizures, monitoring the condition of vital organs, patient care measures, as well as the use of specific therapy methods that stimulate the protective mechanisms of brain tissue in conditions of acute ischemia and hypoxia . The same applies to the processes of correction of chronic forms of cerebral circulatory disorders.
One of the most promising methods of nonspecific therapy for cerebral stroke and chronic forms of cerebral circulatory disorders is currently the use of antioxidants, which are specific correctors of brain energy metabolism, acting specifically under conditions of ischemia and hypoxia.
The body has a physiological antioxidant system that maintains oxidative-antioxidant balance both in liquid media (blood, lymph, intracellular and intercellular fluid) and in the structural elements of the cell (plasmic, endoplasmic, mitochondrial, cell membranes). Enzymatic antioxidants include: superoxide dismutase, which inactivates the superoxide radical inside the cell; catalase, which decomposes intracellular hydrogen peroxide; glutathione dehydroascorbate reductase, some other peroxidases.
Non-enzymatic antioxidants include vitamins C, E, K, glucose, ubiquinones, phenylalanine, transferrin, haptoglobin, tryptophan, ceruloplasmin, carotenoids. Biological and chemically synthesized antioxidants are divided into fat-soluble and water-soluble. The former are localized where the target substrates for attack by free radicals and peroxides are located, the most vulnerable biological structures to peroxidation processes, which include primarily biological membranes, blood lipoproteins, and the main targets in them are unsaturated fatty acids. The most significant fat-soluble antioxidant is α-tocopherol; it interacts with the hydroxyl radical OH and has an inhibitory effect on singlet oxygen, preserving the activity of membrane-bound enzymes. α-tocopherol is not synthesized in the body; it belongs to the group of vitamins (vitamin E), is a universal fat-soluble antioxidant and a natural immunomodulator, normalizing the indicators of cellular and humoral immunity. Among the water-soluble antioxidants, the most important are glutathione, which plays a key role in protecting cells from toxic oxygen intermediates, and the ascorbic acid system, which is especially important for the antioxidant protection of the brain. It should be noted that antioxidants supplied in food also take part in the fight against oxidative stress: minerals (selenium, magnesium, copper compounds), some amino acids, flavonoids (plant polyphenols). However, their role is reduced to a minimum if we take into account that the diet of a modern person is dominated by refined and processed foods that lack natural qualities (even if plant products predominate in the diet), which is the cause of chronic deficiency of antioxidants in the human body.
The most adequate synergist and almost ubiquitous companion of ascorbic acid is the system of phenolic compounds. It is found in all plant living organisms, making up 1–2% of biomass or more, and performs various biological functions.
The antioxidant properties of phenols are associated with the presence in their structure of weak phenolic hydroxyl groups, which easily give up their hydrogen atom when interacting with free radicals and act as free radical traps, turning into low-active phenoxyl radicals. The greatest diversity of chemical properties and biological activity is characterized by phenolic compounds with two or more hydroxyl groups in the benzene ring. Such classes of phenolic compounds form a buffer redox system under physiological conditions. The latest generation phenolic antioxidant is the drug Olifen, the molecule of which contains more than 10 phenolic hydroxyl groups that can bind a large number of free radicals.
Currently, α-tocopherol, ascorbic acid, methionine, cerulloplasmin, carotene, ubiquinone, and emoxypine are used in clinical practice. However, the disadvantage of these drugs is the need for long-term use (several weeks) to ultimately achieve a weak antioxidant and antihypoxic effect. This provided the basis for the search and study of new synthesized antioxidants.
In recent years, the effect of succinic acid, its salts and esters, which are universal intracellular metabolites, has been widely studied. Succinic acid, contained in all tissues and organs, is the product of the 5th and substrate of the 6th reaction of the tricarboxylic acid cycle. The oxidation of succinic acid in the 6th reaction is carried out using succinate dehydrogenase. Performing a catalytic function in relation to the Krebs cycle, succinic acid reduces the concentration of other cycle products in the blood - lactate, pyruvate, citrate, produced and accumulated in the early stages of hypoxia, and is thereby included in energy metabolism, directing the oxidation process along the most economical path. The phenomenon of rapid oxidation of succinic acid by succinate dehydrogenase, accompanied by ATP-dependent reduction of the pool of pyrimidine dinucleotides, is called monopolization of the respiratory chain. The biological significance of this phenomenon lies in the rapid resynthesis of ATP. The Roberts cycle, or the so-called γ-aminobutyrate shunt, functions in nervous tissue, during which succinic acid is formed from γ-aminobutyric acid (GABA) through the intermediate stage of succinic aldehyde. The formation of succinic acid is also possible under conditions of hypoxia and oxidative stress in the reaction of oxidative deamination of α-ketaglutaric acid in the liver. The antioxidant effect of succinic acid is associated with its effect on the transport of mediator amino acids, as well as with an increase in the content of aminobutyric acid in the brain due to the Roberts shunt. Succinic acid in the body normalizes the content of inflammatory mediators histamine and serotonin, increases microcirculation in organs and tissues, primarily in the brain, without affecting blood pressure and heart function. The antihypoxic effect of succinic acid is associated with the activation of succinate dehydrogenase oxidation and the restoration of the activity of cytochrome oxidase, the key redox enzyme of the respiratory chain.
Currently, derivatives of succinic acid are widely used - domestic drugs reamberin, cytoflavin, mexidol.
Mexidol is an antioxidant, membrane protector, antihypoxant with direct energizing action, inhibiting free radicals, reducing the activation of lipid peroxidation, increasing the activity of its own physiological antioxidant system, activating the energy-synthesizing functions of mitochondria and improving energy metabolism in the cell. Mexidol has a modulating effect on membrane-bound enzymes, ion channels, receptor complexes, including GABA and acetylcholine, improves synoptic transmission in brain structures, correcting disorders in microcirculatory systems. Mexidol acts under conditions of ischemia and hypoxia as a specific trap of free radicals, reducing their damaging effect on cerebral structures. The drug is prescribed in doses of 200 to 500 mg per day intravenously in saline or intramuscularly.
Detoxification 1.5% solution for infusion Reamberin, which contains succinic acid salt and microelements (magnesium chloride, potassium chloride, sodium chloride), has antioxidant, antihypoxic, energy-protective effects, reduces the production of free radicals, has a positive effect on aerobic processes during ischemia and hypoxia, restores the energy potential of the cell, utilizes fatty acids and glucose in the cells, normalizes the acid-base balance and gas composition of the blood. Reamberin is successfully used as an infusion solution in critical conditions associated with brain damage, as well as in any conditions caused by endo- and exotoxicosis (cerebral strokes, delirious and predelirious states, poisoning, infectious diseases, clinical manifestations of a systemic inflammatory reaction, liver failure , pancreatic necrosis, peritonitis). The standard dosage is up to 800 ml (400 ml 2 times) per day intravenously. The drug can serve as a basic infusion solution for the use of other medications.
Cytoflavin is a metabolic corrector and energy protector, antioxidant, antihypoxant, aimed at normalizing conditions accompanied by disruption of free radical homeostasis, having a pronounced anti-ischemic effect, reducing the intensity of lipid peroxidation, stimulating the antioxidant defense system. Cytoflavin is a balanced complex of two metabolites (succinic acid, riboxin) and two coenzymes of vitamins - riboflavin (B2) and nicotinamide (PP). The active substances included in this complex preparation have a high level of influence on the metabolism of neuronal structures and act as effective correctors of its imbalance under conditions of ischemia, hypoxia and oxidative stress. Thus, riboflavin mononucleotide, a coenzyme that activates succinate dehydrogenase, a flavoprotein used to activate alternative NAD (Nicotinamide Adenine Dinucleotide)-dependent metabolic pathways, has a direct antihypoxic effect associated with an increase in the activity of flavin reductases and restoration of the level of ATP and creatine phosphate (macroergs). It has been proven that riboflavin penetrates the cell membrane regardless of pH. Its entry into the cell depends only on the value of the transmembrane potential. Riboflavin stimulates the utilization of succinic acid by activating the mitochondrial transport system of dicarboxylic acids of the Krebs cycle through the shuttle (glycerol phosphate) pathway, and succinic acid, in turn, increases the transmembrane potential, increasing the transport of riboflavin across membranes. In addition, riboflavin increases the activity of dehydrogenases, preventing ischemic damage to nervous tissue, and inhibits lipid peroxidation in tissues provoked by iron ions Fe2+.
Riboxin (inosine) has a pronounced antioxidant effect, which is realized by a complex of interconnected metabolic pathways, stimulating the activation of NAD synthesis in mitochondria from nicotinamide and stimulating anaerobic glycolysis with the formation of lactate and NAD. It is characterized by a neuroprotective effect in reperfusion syndrome, potentiating the vasodilating effect of adenosine and inhibiting the enzyme adenosine deaminase.
Nicotinamide is a neuroprotector, one of the fragments of NAD, which activates NAD-dependent cell enzymes, including the antioxidant systems of ubiquinone oxyreductases, which protect cell membranes from destruction by radical particles. Nicotinamide is a selective inhibitor of the enzyme poly-ADP-ribose synthetase, which is formed under ischemic conditions and leads to dysfunction of intracellular proteins with subsequent cell apoptosis.
Succinic acid, as an antioxidant, deactivates peroxidases in mitochondria and increases the activity of NAD-dependent enzymes. Nicotinamide and riboflavin, in turn, increase the pharmacological activity of succinic acid. The drug is administered in a dose of 10–20 ml per day intravenously by slow drip in saline solution or 5% glucose. In severe conditions associated with diffuse hypoxia, resuscitation measures, post-reperfusion syndrome, the dosage of the drug can be increased to 40 ml per day, intravenous slow drip administration (60 drops per minute) is indicated.
Numerous pilot and placebo-controlled studies have revealed the positive effect of including the above antioxidants (cytoflavin, reamberin and mexidol) in the complex therapy of patients with cerebral strokes and chronic forms of cerebrovascular disorders. Research in recent years has shown the feasibility of the complex use of these drugs in the treatment of cerebrovascular disorders, since Mexidol and Cytoflavin have different points of application and their combined use can help correct energy processes in brain tissue with simultaneous utilization of free radical oxidation products.
In addition, cytoflavin has been shown to be highly effective in the treatment of patients with intracerebral hemorrhages, characterized by a particularly high level of oxidative stress. A clear relationship between the effect of cytoflavin therapy and the size of intracerebral hematoma was revealed. When cytoflavin is included in the complex therapy of intracerebral hemorrhages, the most significant regression of disorders of consciousness is observed, especially pronounced in hematomas measuring 10–30 cm3, a more rapid regression of focal neurological deficit, and a better functional outcome.
For all modern antioxidants, a clear dependence of the degree of effectiveness on the timing of initiation of therapy has been proven. The maximum clinical effect can be achieved when therapy is started within a period of 2 to 6 hours from the moment of cerebral catastrophe. A less striking but real clinical effect in the form of activation of consciousness and a decrease in focal neurological symptoms is observed when therapy is started within a period of up to 24 hours.
In patients with chronic ischemia, long-term planned therapy with antioxidants significantly corrects the quality of life and helps prevent the progression of functional and morphological cerebral disorders.
Early therapy with antioxidants is currently considered as a real pathogenetically determined method for correcting cerebral metabolism in cerebral vascular disorders.
S. A. Rumyantseva
,
Doctor of Medical Sciences, Professor A. A. Kravchuk E. V. Silina RGMU, City Clinical Hospital No. 15, Moscow