Functional classification of pulmonary hypertension
| Class I | There is no restriction on physical activity. Ordinary physical activity does not cause shortness of breath, weakness, chest pain, or dizziness |
| Class II | some decrease in physical activity. Ordinary physical activity is accompanied by shortness of breath, weakness, chest pain, dizziness |
| Class III | severe limitation of physical activity. Little physical activity causes shortness of breath, weakness, chest pain, dizziness |
| Class IV | inability to perform any physical activity without the above clinical symptoms. Shortness of breath or weakness may be present even at rest, discomfort increases with minimal exertion |
Interview and examination of the patient
It is necessary to find out whether the patient has had episodes of deep vein thrombosis, sudden swelling of the legs, or thrombophlebitis. Many patients have a family history of sudden death, cardiovascular disease, and an increased tendency to thrombus formation.
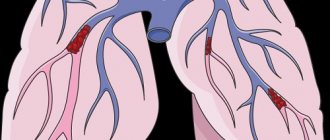
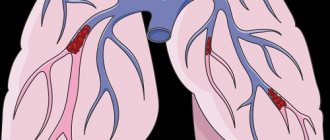
Objective evidence of a history of pulmonary embolism (PE) is the coincidence in time of the clinical presentation of thrombosis of the veins of the lower extremities and the appearance of shortness of breath. In the coming months after PE, a period can be identified in patients when the condition remains stable and asymptomatic. This is due to the fact that the right ventricle copes with the load and allows maintaining good exercise tolerance until progressive pulmonary vascular remodeling develops. Almost the only reliable evidence of previous PE can be data from perfusion scintigraphy or computed tomography of the lungs performed during an acute episode of PE.
During a general examination of patients with CTEPH, blueness (cyanosis) may be detected. With the development of right ventricular heart failure, swollen neck veins, enlarged liver, peripheral edema, and abdominal dropsy are noted.
Modern methods of treatment of pulmonary valve defects
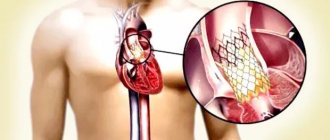
Drug treatment of pulmonary artery defects is aimed at preventing the development and progression of heart failure. Infants with pulmonary atresia are given drugs to prevent closure of the ductus arteriosus until emergency surgery is performed. Surgical treatment, in most cases, can normalize hemodynamics by eliminating the heart defect.
The following operations for pulmonary valve defects are performed at the Herzliya Medical Center Hospital:
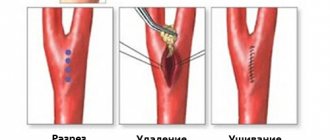
- Percutaneous puncture for pulmonary atresia followed by balloon dilation. The procedure is performed to restore pulmonary perfusion in newborns;
- Balloon expansion of stenosis, stenting and the use of an innovative cutting balloon technique, which allows not only to expand the narrowed area, but also to remove excess fibrous tissue, leading to relapse of stenosis;
- Organ-preserving procedures for the reconstruction of a damaged valve, preventing the need for its replacement;
- Open heart surgery to restore normal patency in atresia and stenosis of the pulmonary trunk;
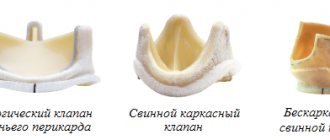
- Pulmonary valve replacement surgery. Artificial biological or mechanical valves fully cope with their function, guaranteeing the restoration of hemodynamics for many years.
Innovative technologies of open and minimally invasive cardiac surgery, widely introduced at Herzliya Medical Center, have changed the prognosis of severe heart defects. Thanks to the combination of experienced surgeons, excellent hospital conditions, highly professional post-operative care and intensive rehabilitation therapy, thousands of patients from all over the world have been restored to a full and active lifestyle.
Non-invasive diagnostics
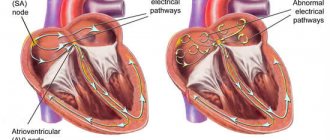
Electrocardiography (ECG) reveals signs of hypertrophy and overload of the right ventricle, dilatation and hypertrophy of the right atrium (p-pulmonale), deviation of the electrical axis of the heart to the right.
Chest X-ray allows you to clarify the etiology of PH: identify interstitial lung diseases, acquired and congenital heart defects, and also judge the severity of PH. The main radiological signs of PH are bulging of the trunk and left branch of the pulmonary artery, which form the second arch in the direct projection along the left contour of the heart, expansion of the roots of the lungs, and enlargement of the right parts of the heart. In patients with post-embolic pulmonary hypertension, signs can be identified that indicate the presence of blood clots in the large branches of the pulmonary artery (PA) - dilation of the trunk and main branches of the PA, a symptom of deformation and shortening of the root. A specific symptom is the depletion of the pulmonary pattern in the area of impaired blood supply.
Echocardiography (EchoCG) - Ultrasound of the heart is considered the most valuable non-invasive method for diagnosing PH, as it not only allows one to assess the level of pressure in the pulmonary artery, but also provides important information about the cause and complications of PH. Using this method, it is possible to exclude damage to the mitral and aortic valves, myocardial disease, congenital heart defects with blood shunting, leading to the development of PH. Unfortunately, the method does not allow differentiating post-embolic pulmonary hypertension from other forms of precapillary PH. The exception is rare cases of the presence of massive thrombi in the trunk and main branches of the pulmonary artery in the immediate vicinity of the bifurcation.
Degrees of heart defects in a child
Depending on the severity of the symptoms of heart disease, there are four degrees of impairment:
- first degree
- heart function deviates slightly from the norm; - second degree
- symptoms of the disease appear, parents can notice them; - third degree
- in addition to specific symptoms, disturbances in the functioning of the nervous system appear, as a result of a lack of oxygen to the brain; - fourth degree
- respiratory and cardiac activity is inhibited, such changes can lead to the death of the child.
Establishment of clinical class and verification of diagnosis
Pulmonary function tests can identify obstructive or restrictive changes for the purpose of differential diagnosis of PH and clarify the severity of lung damage. Patients are characterized by a decrease in the diffusion capacity of the lungs for carbon monoxide (40-80% of normal), a slight or moderate decrease in lung volumes, a normal or slightly decreased PaO2, and usually a decreased PaCO2 due to alveolar hyperventilation.
Ventilation-perfusion lung scintigraphy is a screening method to exclude chronic thromboembolism as a cause of pulmonary hypertension. In patients after thromboembolism, perfusion defects are found in the lobar and segmental zones in the absence of ventilation disturbances. Perfusion scintigraphy has historically become one of the first methods for detecting perfusion defects in the pulmonary parenchyma in pulmonary embolism. The images obtained in acute PE and CTEPH differ significantly. Perfusion defects in acute PE are more clearly defined and contrast sharply with normally functioning tissue. In CTEPH, perfusion defects are not clearly defined and often do not correspond to the blood supply area of the large pulmonary artery.
Computed tomography and CT angiopulmonography
The CT picture of chronic thromboembolism can be represented by occlusions and stenoses of the pulmonary arteries, eccentric filling defects due to the presence of blood clots, including recanalized ones. CT angiopulmonography is performed on spiral computed tomographs during the phase of passage of the contrast agent through the pulmonary arterial bed. Among the methodological features, it should be noted that the study must be carried out using at least an 8-spiral tomograph, with a minimum step (no more than 3 mm) and a slice thickness (no more than 1 mm). A thorough scan should cover both lungs completely, from the apices to the phrenic sinuses. Contrast enhancement of the right chambers of the heart and pulmonary arteries should match or exceed the degree of contrast enhancement of the left chambers of the heart and aorta. The second, arterial phase of scanning is recommended for all patients over 40 years of age, especially if there is evidence of arterial thrombosis and coronary artery disease in the anamnesis. Modern software allows you to reconstruct images of the pulmonary arteries in any plane, construct maximum intensity projections and three-dimensional images. In most cases, to clarify the nature of the lesion, it is enough to analyze cross sections using an image viewer, which makes it possible to determine the presence of changes not only in the lobar and segmental branches, but also in a number of subsegmental arteries. Pathological changes, in addition to the presence of “old” thrombotic material, may include local thickening of the vessel wall, narrowing at the mouth of the vessels and along them, occlusions, intravascular structures in the form of membranes and bridges. If changes are detected in several branches of the pulmonary arteries, we can conclude that there is a high probability of thromboembolic nature of PH. It is important to note that the resolution of modern CT scanners is limited and does not allow the determination of very thin membranous and stringy structures in the lumen of the LA, especially if the size of the object does not exceed 2-3 mm. In some cases, calcification of the “old” thrombotic material develops, and CT can be invaluable in determining the location of the calcification. CT makes it possible to detect not only stenotic changes in the vessels of the lungs, but also disturbances in the perfusion of lung tissue by the nature of the contrast of the parenchyma. In some cases, parenchymal enhancement is so uneven that mosaic enhancement is detected on scans. A clearly defined mosaic pattern of segments usually indicates a good prognosis for surgical treatment. Contrasting exclusively in the root zones is not a true mosaic and is often observed in microvascular forms of PH. By providing detailed images of the lung parenchyma, CT allows the diagnosis of other lung diseases. In addition to the state of the arterial bed, CT can provide comprehensive information about all intrathoracic structures, which is important for confirming the diagnosis and developing a surgical treatment plan. Before performing the operation, the condition of the pulmonary parenchyma, bronchial tree, and pulmonary veins should be taken into account.
Angiographic diagnostics
The main objectives of angiographic diagnosis are to determine the severity of pulmonary hypertension, clarify the nature of the lesion in the pulmonary bed through angiopulmonography, and identify/exclude coronary disease. Carrying out catheterization in isolation without high-quality angiopulmonography in a patient with clear signs of CTEPH is inappropriate. This study should provide clear information to doctors to resolve the issue of the patient’s operability and the severity of his condition. Hemodynamic criteria for post-embolic pulmonary hypertension, identified during catheterization of the right heart, are: mean pulmonary artery pressure (PAP) above 25 mm Hg. Art., pulmonary artery wedge pressure (PAWP) ≤ 15 mm Hg. Art., PVR > 2 units. according to Wood (160 dyn. sec cm-5) in the presence of multiple stenotic and/or occlusive lesions of the branches of the pulmonary artery of various calibers.